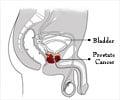
Research has indicated that a new test could reliably detect early increases in prostate specific antigen (PSA) levels in men who have undergone prostate cancer-treating surgery.

Data measuring the efficacy of this new test were presented at the Fourth AACR International Conference on Molecular Diagnostics in Cancer Therapeutic Development.
"AccuPSA is a simple blood test that can tell a physician important information about prostate specific antigen levels after radical prostatectomy," said David Wilson, Ph.D., senior director of product development at Quanterix Corporation, the manufacturer of the test. "AccuPSA has the potential to eliminate unnecessary treatments and enable earlier detection of recurrence, which may lead to earlier treatment, better outcomes and have a positive impact on health care costs."
After undergoing radical prostatectomy, many men remain at a significant risk for cancer recurrence. Because of this, patients are monitored very closely for rapid increases in PSA, which may signal cancer recurrence.
Standard PSA tests are primarily used to screen asymptomatic men for prostate cancer. However, once the prostate is surgically removed, PSA levels are usually undetectable using standard tests, according to Wilson. AccuPSA, which uses Quanterix's proprietary Single Molecule Array (SiMoA™) technology, is able to detect PSA with unprecedented sensitivity, and at much lower levels than standard PSA tests because it can selectively capture and measure individual PSA molecules.
To determine the accuracy of the novel blood test, PSA levels were measured in blood taken from 60 men who had undergone radical prostatectomy. These specimens had all been categorized as being below the detection limit of standard PSA tests. However, using AccuPSA, researchers were able to measure PSA in all of the samples.
The next step in this research is to conduct a large retrospective clinical study to formally establish the utility of this test.
Source-Eurekalert
 MEDINDIA
MEDINDIA
![Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis](https://images.medindia.net/patientinfo/120_100/prostate-specific-antigen.jpg)
 Email
Email