Peripheral vascular disease patients may not benefit from aspirin therapy, finds a recent study from the University of Florida.
TOP INSIGHT
Aspirin therapy may not provide any cardiovascular benefits for patients with peripheral vascular disease.
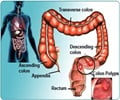
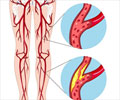
Aspirin prevents blood clots from forming, which can reduce the risk of a stroke or heart attack. But it can also be a hazard: Blood that doesn't clot easily can raise the risk of a hemorrhagic stroke or internal bleeding. Approximately 8.5 million people in the United States have peripheral vascular disease including up to 20 percent of those over age 50, according to the Centers for Disease Control and Prevention.
Among the major findings from the analysis: After about six years, 7.7 percent of PVD patients who took aspirin had died, compared with 8.5 percent in a control group. The incidence of stroke was 3.2 percent among aspirin users and 4 percent among non-users. Heart attacks were recorded in 3.5 percent of aspirin users and 5.5 percent of non-users.
However, all differences did not reach statistical significance with overlapping confidence intervals. The prevalence of other major adverse cardiac and cerebrovascular events was similar among both groups.
The mean age of patients included in the analysis was 62. Sixty percent of the patients were women, 32 percent were people with diabetes and 67 percent were current or ex-smokers.
While noting that the analysis is not the final word on aspirin's effectiveness in PVD cases, the researchers said it is the most updated analysis that compares medical outcomes among those who use aspirin and those who do not. Among other factors, the analysis was limited by the large weight given to a single trial and the fact that many of the trials were done before cholesterol-reducing medications were common. Larger, randomized trials will be needed to confirm the findings that were revealed in the analysis, said Ahmed N. Mahmoud, M.D., a cardiology fellow in the department of medicine and a co-author of the study.
Patients who are on a daily aspirin regimen for cardiovascular issues should not stop taking the medicine on their own but can consult their physician about whether the current findings may be relevant, Bavry said. For cardiologists and researchers, Bavry said the analysis underscores the need for further study. A study to assess aspirin's risks and benefits in patients' conditions such as stable ischemic heart disease, which stems from plaque buildup in arteries, is also underway, he added.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email