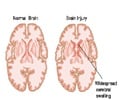
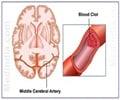
Blood clot in the brain causes Thromboembolic stroke, resulting in damage to the parts of the brain deprived of oxygen.
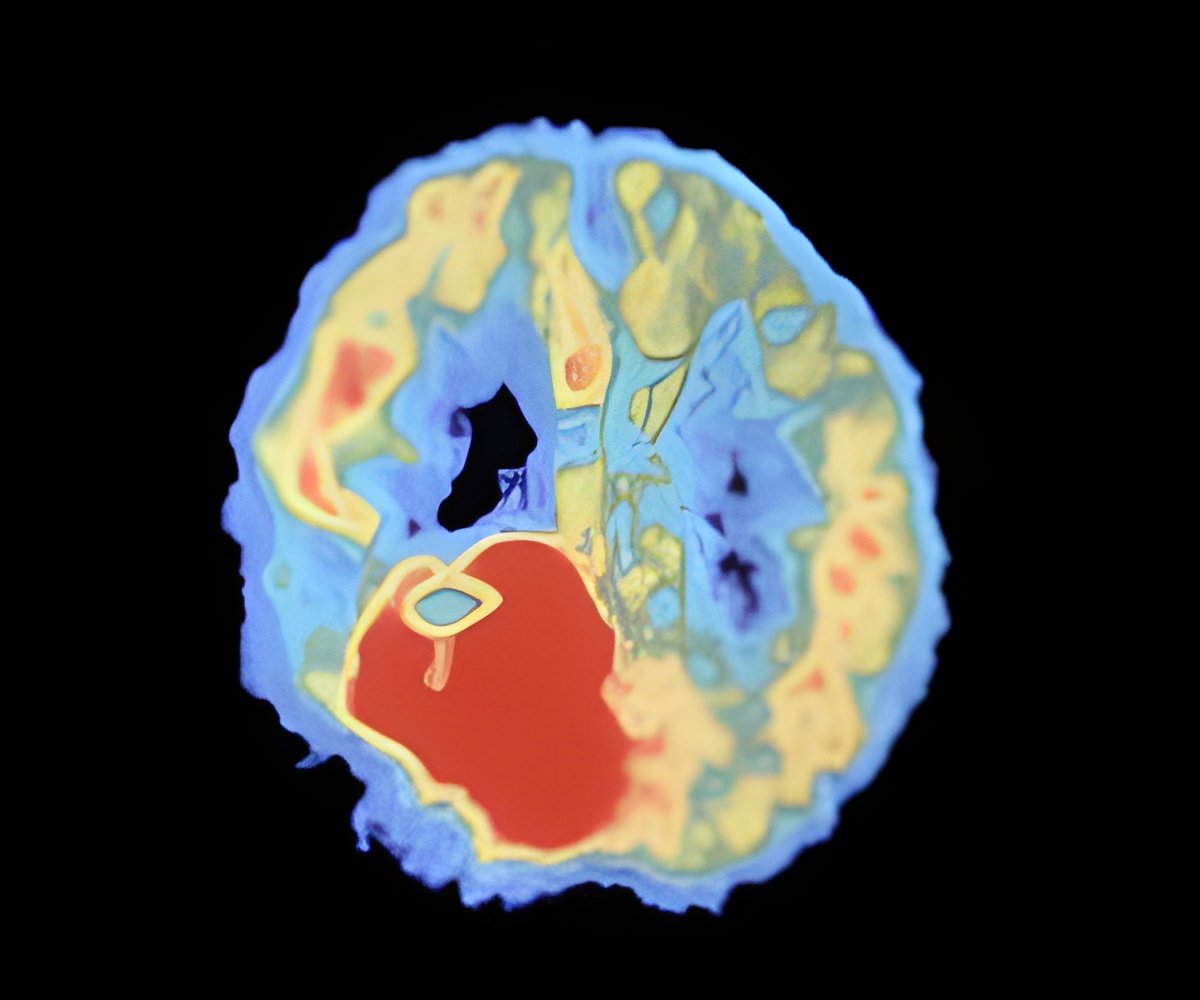
Mild hyperthermia is known to be neuroprotective and to reduce damage caused by the return of blood flow to an area of the brain starved of oxygen by a clot. Researchers from the University of Erlangen, led by Dr Rainer Kollmar, tested whether mild hyperthermia could also prevent damage to the brain due to tPA treatment in rats. After 24 hours they found that, while hypothermia reduced the amount of swelling and damaged tissue in the brain after a stroke, tPA (administered 90 minutes after the onset of stroke) increased it. However, they also discovered that hypothermia therapy was able to offset the damage due to tPA.
This seemed to be true for all the measurements they looked at. Dr Kollmar explained, "Patients often loose brain function such as control over parts of their body, speech or memory after stroke. We looked at 'neuroscore', to examine how much control of the body had been affected, and at markers for inflammation (TIMP-1 and sICAM) or evidence of damage to the blood brain barrier. In all cases hypothermia was able to offset the side effects of tPA."
While these results are still experimental, new techniques which prevent shivering mean that this technique is easier to administer in conscious patients. Preliminary clinical trials are also beginning to show that it is possible to treat patients, who have had a stroke, with tPA plus hypothermia. Our results suggest that hypothermia can offset the side effects of tPA and further studies will show if it is also able to increase the window of opportunity of tPA treatment in patients.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email