Induced pluripotent stem cells are cells that have the potential to regenerate any cell or tissue in the body.

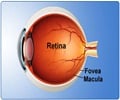
‘Successful transplantation of retinal pigment epithelium (RPE) cells will depend upon repair of the damaged Bruch's membrane beneath the cells.’





"This works because the DNA ultimately leads to creation of a protein inside the cell, which then affects the cell’s behavior," explains Del Priore.The efficiency is low; only about 1% of cells become transformed, he reports, but the research establishes that these cells can then be turned into RPE and that these cells function normally in the Petri dish.
Specifically, the work demonstrates that the generated RPE can ingest outer segments from the retina, which is important in the normal maintenance of this delicate neural tissue. Work on this project involved a collaborative research team that included Ernesto Moreira, Mark Fields, and Zsolt Ablonczy.
Successful transplantation of RPE cells will depend upon repair of the damaged Bruch’s membrane (BM) beneath the cells, and Del Priore and investigators also have reported on the effects of doing a "chemical peel" of this substrate in Translational Vision Science and Technology (Oct 30, 2015).
BM explants were dissected from young and old donor eyes. A combination of cleaning and then coating the explants with extracellular matrix ligands removed the abnormal protein deposits and rejuvenated the tissue. These results demonstrate that the detrimental effects of aging BM can be reversed by reengineering the BM surface with this approach.
Advertisement
Advertisement