Inflammation, the body's response to injury, seems to be the key connection between fat, bacteria and diabetes

Senior author Patrick Schlievert, Ph.D., UI professor and head of microbiology, said that the idea is that when fat cells (adipocytes) interact with environmental agents-in this case, bacterial toxins-they then trigger a chronic inflammatory process.
The researchers used immortalized fat cells to show that bacterial toxins stimulate fat cells to release molecules called cytokines, which promote inflammation.
Co-senior author of the study Al Klingelhutz, Ph.D., UI microbiologist, said that by immortalizing fat cells the UI team created a stockpile of continuously dividing, identical cells that are necessary for repeat experiments to validate results.
The UI team focused on a different bacterium, Staphylococcus aureus (staph), which appears to be important in the context of diabetes for two reasons. First, as people become obese and then progress into diabetes they become very heavily colonized with staph bacteria.
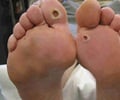
Secondly, staph is the most common microbe isolated from diabetic foot ulcers, one of the most common and health-threatening complications of diabetes.
The new UI study shows that superantigens from staph bacteria trigger fat cells to produce pro-inflammatory molecules. Moreover, the study found that superantigens synergized with LPS from E. coli to magnify fat cells' cytokine responses, amplifying the inflammation, which could potentially boost the likelihood of developing diabetes.
Source-ANI
 MEDINDIA
MEDINDIA

 Email
Email