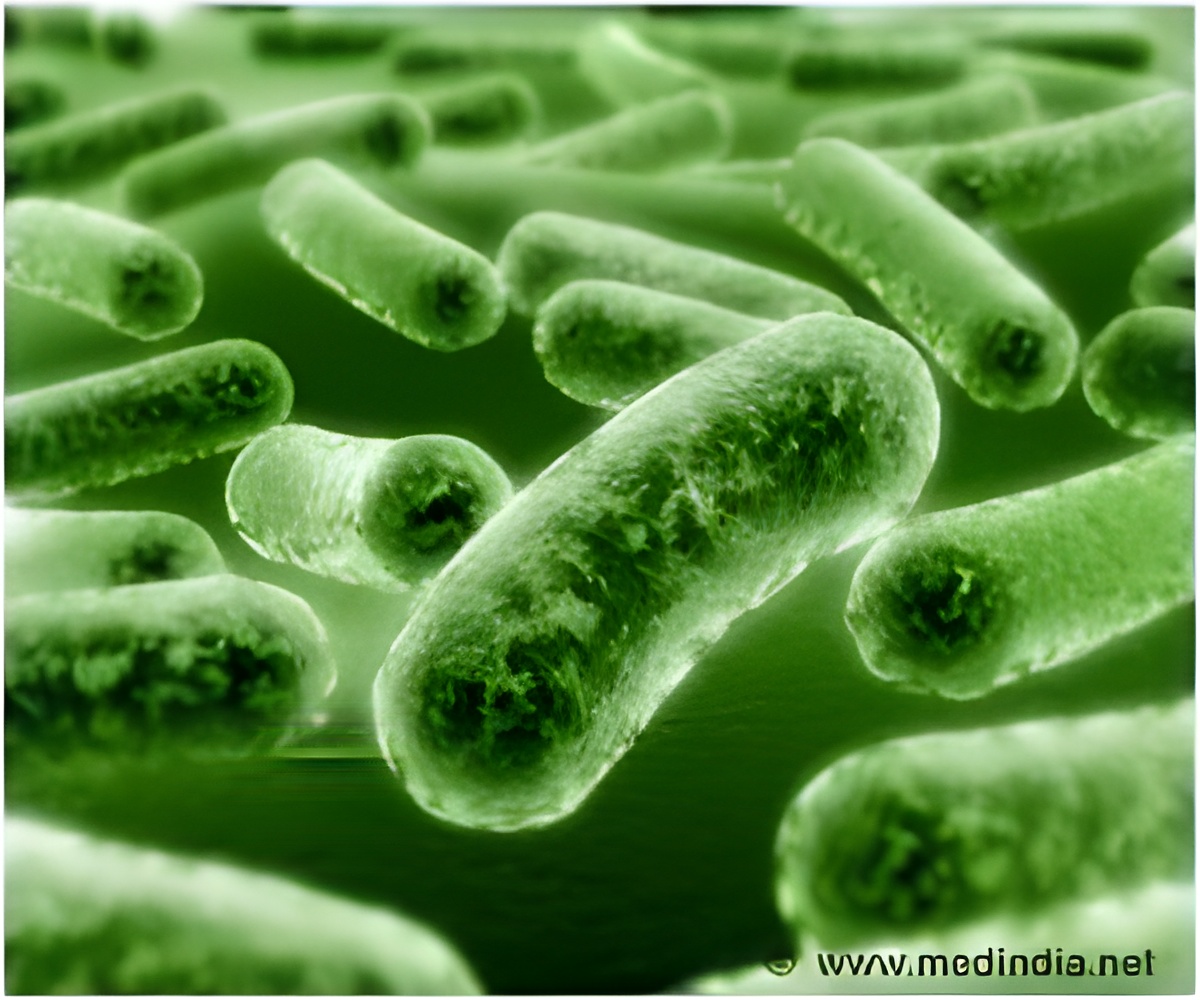
Frequent consumption and misuse of antibiotics make the bacteria become multi-drug resistant and recolonizes in the body when the treatment is stopped.
TOP INSIGHT
A daily dose of antibiotics kills most of the bacteria. But, some bacteria remain dormant and becomes active when the treatment is stopped.
To examine this phenomenon in detail, researchers from the KU Leuven Centre of Microbial and Plant Genetics treated the gut bacteria Escherichia coli with a daily dose of antibiotics in the lab.
Most of the bacteria were initially killed. But, some bacteria found a quick way to adapt with minimal changes in their genetic material.
The result was the rapid development of many persister cells. These cells are in a dormant state, and, therefore, are insusceptible to the antibiotic treatment. These bacteria survive the antibiotic treatment and can resume their reproduction after the treatment.
These tolerant cells can just sit out treatment, says Professor Michiels. “On the first day of treatment, they are already present, albeit in small numbers. They ensure that the population is not wiped out and that it can be reconstituted after the antibiotic treatment. Eventually, you end up with an entire population that is tolerant to several antibiotics.”
The researchers also noted that the number of cells with multi-drug tolerance decreases again as soon as the antibiotic treatment is stopped.
Currently, the researchers are examining whether other pathogens show a similar increase in tolerance and whether genetic adaptation takes place during the treatment of infections in human beings.
Source-Medindia
 MEDINDIA
MEDINDIA


 Email
Email










