Damien J. LaPar, MD, MSc, of the Division of Thoracic and Cardiovascular Surgery at the University of Virginia (Charlottesville), is presenting the results of this research at the 94th AATS Annual Meeting in Toronto, ON, Canada on April 30, 2014.
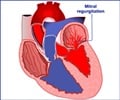
When the mitral valve (MV) leaks, blood can flow backward or "regurgitate" into the upper heart chamber, leading to decreased blood flow to the rest of the body. To compensate, the heart may try to pump harder, and this can result in congestive heart failure. When regurgitation is severe, the standard of care treatment is MV surgery. Two options are available: mitral value repair or replacement.
Professional associations such as the American College of Cardiology and the American Heart Association recommend mitral valve surgery over medical management for severe mitral regurgitation. Yet, only 50% of patients meeting the ACC/AHA guidelines for surgical treatment undergo surgery. Furthermore, while MV repair is associated with superior perioperative outcomes and reduced mortality compared to replacement, it appears to be underutilized.
In this large, multi-institutional retrospective study from the Virginia Cardiac Surgery Quality Initiative, more than 4,000 patients were evaluated, and 60% underwent MV repair. Significant variations were seen in MV repair rates among hospitals (35-70% of MV procedures) and surgeons (0-90%).
The results suggest that what type of surgery a patient received depended in part on how experienced the surgeon was. After adjustment for baseline preoperative patient risk, when the propensity to perform an MV repair was plotted against surgeon volume, it became apparent that there was an "inflection point" of increased probability for mitral repair when the average annual surgeon volume (a surrogate for surgeon experience) exceeded approximately 20 surgeries a year. Surgeons who performed more than 20 MV surgeries a year were between 3 and 4 times more likely to perform a repair than replacement compared to those who operated less than 20 times a year.
Advertisement
Source-Newswise