Early-stage human clinical trials showed that a new topical drug was safe and had biological effects in a type of diabetic eye disease, and may offer researchers a new approach to prevent and treat diabetic macular edema.
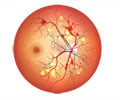
Researchers at the Wilmer Eye Institute of Johns Hopkins University School of Medicine in Maryland completed a multicenter human clinical trial treating diabetic macular edema with mecamylamine, a topical drug developed by the South San Francisco biotech company CoMentis, Inc. Funding for the study was provided by the Juvenile Diabetes Research Foundation (JDRF) through its Industry Drug Development Partnership program. The results were published in the American Journal of Ophthalmology.Diabetic macular edema is a complication of a specific region of the retina in the eye, called the macula, that develops when small blood vessels become leaky such that fluid accumulates. Without treatment, diabetic macular edema can cause vision impairment, blurriness, or blindness. Therapies to free people from the devastating health burden of complications that can accompany diabetes, including diseases of the eye, nerves, and kidneys, are an important focus of JDRF research; in the last fiscal year, the foundation invested more than $22 million in research involving Complications Therapies.
In the Johns Hopkins study, participants with diabetic macular edema were asked to give themselves mecamylamine eye drops twice a day for 16 weeks. (Preclinical research with diabetic mice showed that mecamylamine had the ability to stop the process that contributed to the development and progression of diabetic macular edema.) Based on these preclinical results, the researchers at Hopkins were interested in measuring both the safety and efficacy of this drug in patients. Every four weeks, trial participants met with researchers to receive a complete eye exam to monitor and track changes to the eye.
At the conclusion of this study, approximately 40% of the participants showed significant improvement in overall vision and/or the thickness of the retina. The treatment also showed biological effects in the retina indicating that the drug was able to gain access to the retinal vessels after topical application to the eye. Peter Campochiaro, M.D., professor of ophthalmology at the Johns Hopkins University School of Medicine and principal investigator of the study.
In the study participants, approximately 40% showed no change, and about 20% developed worsening of the condition. The variation in response to the treatment supports the observation that drugs and therapies have less than a 100% response rate, likely due to genetic make-up or unknown factors about the disease. These results also emphasize the notion that multiple treatment options for diabetic macular edema must be explored to compliment current research in this field.
"The safety and early signals of treatment effect arising from this study may create a strong interest in the development of multiple treatment options that are affordable and can be self-administered, helping to ease the burden of healthcare delivery and compliance," said Barbara Araneo, Director of Complications Research for JDRF.
Advertisement
SRM