- Truncus Arteriosus - (http://www.chfed.org.uk/how-we-help/information-service/heart-conditions/truncus-arteriosus/)
- About Truncus Arteriosus - (https://medlineplus.gov/ency/article/001111.htm)
- Future Pregnancy After CHD Diagnosis: 3 Things To Know - (http://blog.cincinnatichildrens.org/rare-and-complex-conditions/heart-conditions/future-pregnancies-after-chd-diagnosis-3-things-to-know/)
- What is Truncus arteriosus? - (https://my.clevelandclinic.org/health/articles/truncus-arteriosus)
- Facts about Truncus Arteriosus - (https://www.cdc.gov/ncbddd/heartdefects/truncusarteriosus.html)
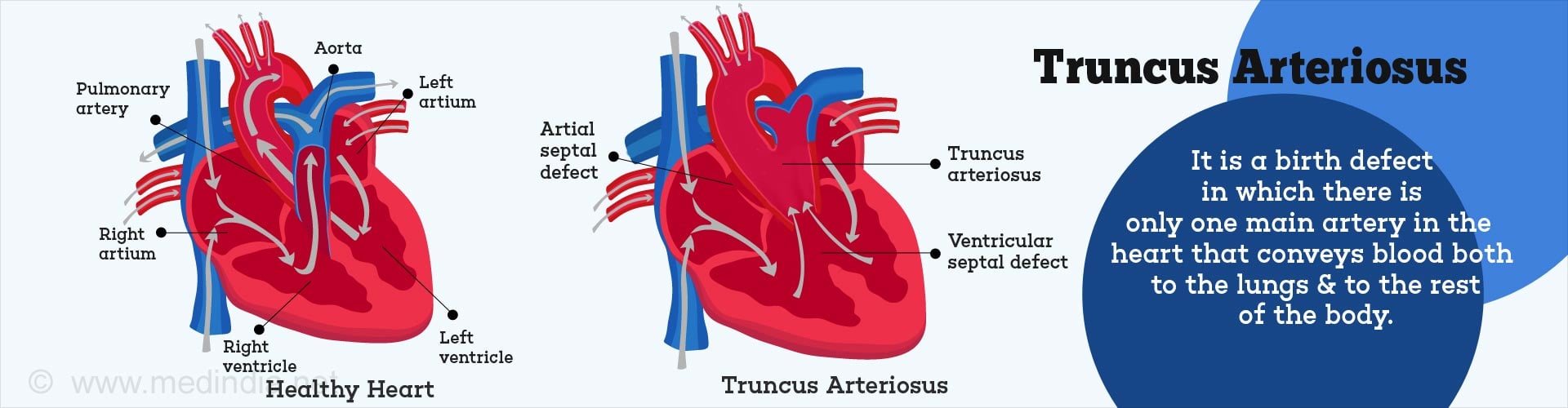
What is Truncus Arteriosus?
Truncus arteriosus is a developmental defect of the heart where there is only a single artery in the heart that carries blood both to the lungs and the rest of the body instead of two separate vessels, one to the lung (pulmonary artery) and the other (aorta) to the rest of the body.
The incidence of truncus arteriosus is about 1 in 10,000 births.
Overview of Blood Circulation
The heart is a four-chambered organ consisting of two atria and two ventricles that work constantly to keep the blood circulation going. The blood circulation is described briefly below in the following steps though it is in fact a continuous process.
- The impure or venous blood from all over the body returns to the right atrium (RA).
- This venous blood then flows into the right ventricle (RV) via the tricuspid valve.
- From the RV, the deoxygenated blood is carried into the lungs via the pulmonary artery (PA) to be purified and oxygenated.
- The pure oxygenated blood is emptied into the left atrium (LA) and reaches the left ventricle (LV) via the bicuspid valve.
- The LV contracts to empty this blood into the major blood vessel, the aorta to be distributed to all the organs and tissues of the body.
Thus, there are two arteries in the heart, the pulmonary artery that conveys venous blood to the lungs and the aorta that distributes oxygenated blood to the entire body.
In truncus arteriosus, the only single large vessel that is present divides itself into the pulmonary and the aortic arteries.
In addition, this defect is associated with a hole in the wall between the right and the left ventricles (the 2 lower chambers), referred to as ventricular septal defect (VSD). As a result, impure blood from the right side mixes with oxygenated blood on the left side of the heart, which is then carried to the lungs and also the rest of the body via the truncus.
What are the Types of Truncus Arteriosus?
Depending on the branching pattern of the pulmonary artery, truncus arteriosus is classified into the following types described by Collett /Edwards 1949.
- Type 1 - Pulmonary artery branching takes place just above the valve.
- Type 2 - Pulmonary arteries branching to the lungs is separate but close together directly off the truncus.
- Type 3 - Pulmonary arteries branch separately and are far apart.
What are the Causes of Truncus Arteriosus?
The exact etiology is not known. However there have been several risk factors associated with the development of this condition, which occurs in the womb during fetal development. The risk factors include the following:
- Family history of congenital heart disease
- German measles (rubella), a viral illness during pregnancy
- Poorly controlled diabetes in the pregnant woman
- Smoking and alcohol during pregnancy
- Chromosomal disorders – Babies with Di George’s syndrome, velocardiofacial syndrome appear to be at increased risk of developing truncus arteriosus
- Certain medications taken during pregnancy are associated with defective heart development, for example antiseizure drugs and Ibuprofen

What are the Symptoms of Truncus Arteriosus?
In truncus arteriosus there is too much blood going into the lungs than would in a normal newborn. In addition, when there is associated VSD as is often the case, there is mixing of pure and impure blood. Signs and symptoms are evident within a few days after birth and include the following:
- Shortness of breath (dyspnea)
- Rapid shallow breaths (tachypnea)
- Bluish discoloration of skin (cyanosis)
- Poor feeding
- Weak cry
- Failure to gain weight or thrive
- Irregular heart beat

How do you Diagnose Truncus Arteriosus?
History and Physical Examination:
- When the anxious parents and family members consult the pediatrician or child specialist, he will obtain a detailed history and perform a thorough physical examination, which will reveal the above signs and symptoms and raises suspicions of a heart defect.
- In addition a chest examination may show the presence of abnormal heart sounds or murmurs and may also point to presence of fluid in the lungs.
He may order some blood tests and imaging to determine the cause.
Blood tests:
- Testing of the baby’s blood (pulse oximetry, a simple bedside test) may show low levels of oxygen saturation responsible for the breathlessness and bluish discoloration of skin and mucous membranes.
Imaging tests:
- Chest x-ray – A chest x-ray may show evidence of fluid accumulation in the lungs and outline the size of the heart.
- Echocardiogram – An echocardiogram is essentially an ultrasound scan of the heart and reveals the activity of the heart as an image.
- The presence of a single large vessel leading from the heart, the defect in the wall between the left and right ventricles, and other abnormalities in the valve between the large vessel and the ventricles are seen. The amount of blood flowing into the lungs and the risk for developing high blood pressure in the pulmonary vessels (pulmonary hypertension) can also be determined.
- CT and MRI Heart – These investigations give more detailed information and a clearer picture of the heart compared to a plain chest x-ray.
- Cardiac catheterization – This is procedure that involves the introduction of a thin flexible tube into the heart through a blood vessel in the groin and injecting a contrast agent. Detailed imaging of the heart vasculature is obtained.
How do you Treat Truncus Arteriosus?
Surgery is the definitive treatment, usually performed in the neonatal period (1-2 weeks after birth).
Medications:
Before the surgery is performed, the child may receive medications such as diuretics and digoxin to improve heart and lung function. Digoxin improves the strength of heart muscle contractions, and enables it to pump more efficiently. Diuretics help remove extra fluid from the lungs and body, which often occurs in cases of heart failure.
Surgery:
- During the surgery, the ventricular septal defect (hole in the wall between the right and left ventricles) is closed with a patch.
- The upper part of the pulmonary artery is separated from the single common artery (truncus arteriosus) and connected with the right ventricle using a tube or a conduit.
- The single large vessel is then reconstructed to create a new aorta. The surgeon might also repair the truncal valve, if necessary.
What are the Complications of Truncus Arteriosus?
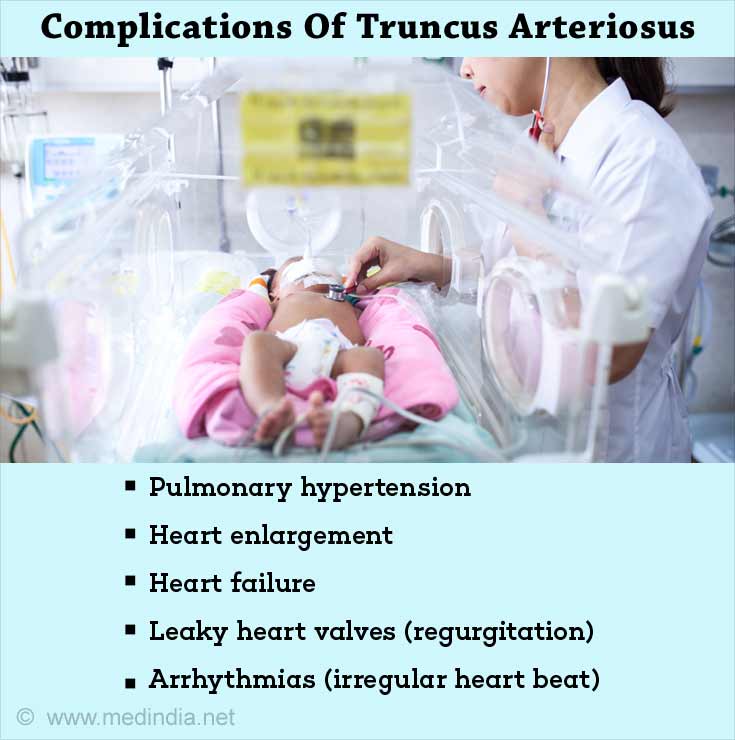
Complications associated with truncus arteriosus include the following:
- Pulmonary hypertension – This occurs due to increased blood flow in the lungs, which causes the pulmonary vessels to reflexly constrict causing raised pressure in the pulmonary circulation.
- Heart enlargement (cardiomegaly) – The presence of pulmonary hypertension, and increased blood flow through the heart makes the heart pump harder causing enlargement and thickening of its walls.
- Heart failure – This can result due to reduced oxygen supply to the heart and due to increased workload on the heart.
- Leaky heart valves (regurgitation).
- Arrhythmias (irregular heart beat).
How do you Prevent Truncus Arteriosus?
As mentioned previously, certain risk factors are associated with the development of congenital heart defects. These can be addressed to reduce or prevent the development of heart defects.
- Avoid taking medications during pregnancy without the consent of your doctor. Some of the drugs known to be associated with an increased incidence of congenital heart defects include benzodiazepines, lithium, acne medications such as isotretinoin and topical retinoids and the non-steroidal anti-inflammatory (NSAID) drug Ibuprofen. Paracetamol is a safer alternative during pregnancy.
- Avoid smoking and alcohol intake during pregnancy.
- Get vaccinated against specific viral illnesses especially rubella which is known to cause fetal heart defects. Flu illness is also known to cause birth defects in the heart. It is recommended that pregnant women take the flu shot.
- Controlling diabetes, as uncontrolled hyperglycemia can affect the fetus in several ways.
- Taking folic acid 400 mcg once daily during pregnancy might help prevent the development of neural tube defects and possibly fetal heart abnormalities.