- Rapid sequence spinal anaesthesia for category-1 urgency caesarean section: a case series - (https://pubmed.ncbi.nlm.nih.gov/20642523/)
- Combined Spinal-Epidural Anesthesia - (https://www.nysora.com/topics/regional-anesthesia-for-specific-surgical-procedures/abdomen/combined-spinal-epidural-anesthesia/)
- Continuous spinal anesthesia with epidural catheters: An experience in the periphery - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4173398/)
- Segmental Spinal Anesthesia: A Systematic Review - (https://www.longdom.org/open-access-pdfs/segmental-spinal-anesthesia-a-systematic-review.pdf)
- Subarachnoid Block (also Known As Spinal Block) - (https://resources.wfsahq.org/atotw/subarachnoid-block-also-known-as-spinal-block/)
What is Spinal Anesthesia?
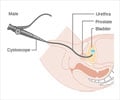
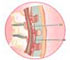
Spinal anesthesia is a form of neuraxial regional anesthesia that involves the injection of an anesthetic drug into the subarachnoid space, which is a fluid-filled space in which the spinal cord and the nerves arising from it are suspended. The drug then mixes with the cerebro-spinal fluid and acts on the nerve fibers, blocking their activity for a finite time. This renders the portion of the body below the level of the injection numb and anesthetized while the rest of the body remains active.
This fluid-filled space is called the subarachnoid space, and the injection is most commonly given in the region of the lumbar (low back) spine. Hence a spinal block is technically a subarachnoid block or intrathecal block. The block is performed using a special spinal needle. This form of regional anesthesia is easy to administer and is ideally suited for surgeries performed in the lower parts of the body, like Caesarean sections during pregnancy and lower limb and abdominal surgeries. The first operation under spinal anesthesia was performed in 1898 in Germany by August Bier.
Spinal Anesthesia: Types and Techniques
The administration of spinal anesthesia requires appropriate positioning and an understanding of neuraxial anatomy. As mentioned earlier, spinal anesthesia is performed in the lumbar area, specifically the mid-to low-lumbar level. This is done to avoid damage to the nerves exiting from the spinal cord. The level of blockade hence depends on the level at which the drug is given, the type of drug based on drug density, drug volume, and the position of the patient after the block is given.
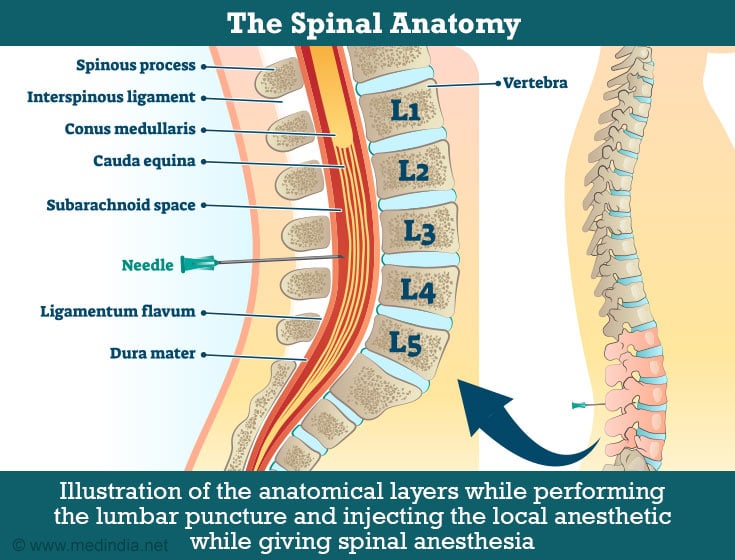
There are a few techniques and modifications for spinal anesthesia.
- Rapid Sequence Spinal Anesthesia: Rapid sequence spinal anesthesia (RSS) is a recently developed technique for the most urgent cases, mainly
Cesarean sections . This consists of a no-touch spinal technique and other technical considerations, along with being prepared for conversion to general anesthesia if there are delays or problems(1✔ ✔Trusted Source
Rapid sequence spinal anaesthesia for category-1 urgency caesarean section: a case series
Go to source). - Combined Spinal and Epidural Anesthesia (CSE): The combined spinal-epidural (CSE) technique, is a comparatively new anesthetic choice that includes an initial spinal block followed by epidural catheter placement. This allows for rapid relief of pain and the subsequent administration of medications for prolonged anesthesia(2✔ ✔Trusted Source
Combined Spinal-Epidural Anesthesia
Go to source). - Continuous Spinal Anesthesia: Continuous spinal anesthesia is the technique of initiating and maintaining spinal anesthesia with small doses of local anesthetic injected intermittently into the subarachnoid space(3✔ ✔Trusted Source
Continuous spinal anesthesia with epidural catheters: An experience in the periphery
Go to source). - Segmental Spinal: Spinal Anesthesia is a modification in which spinal anesthesia is performed by using a subarachnoid puncture at a vertebral level as close as possible to the innervation of the operative field(4✔ ✔Trusted Source
Segmental Spinal Anesthesia: A Systematic Review
Go to source).
Indications of Spinal Anesthesia
- Surgeries below the level of the umbilicus; examples are genitourinary surgery, gynecological surgery, hernia repairs, and surgeries performed on the lower extremities.
- It is especially suited for older patients and those with diseases such as chronic respiratory, renal, or hepatic disease.
- Diabetics also face an advantage from spinal anesthesia.
- It is also suitable in cases of trauma where there is a need for emergency surgery(5✔ ✔Trusted Source
Subarachnoid Block (also Known As Spinal Block)
Go to source).
Spinal Anesthesia: Procedure
- Patient Position: The patient is usually positioned in a sitting posture on the operating table. A small stool for placing the foot can be given for the patient’s convenience and support. The forearms can be made to rest on the thighs to make the patient stable and comfortable.Alternatively, the procedure can be performed with the patient lying on their side with their hips and knees maximally flexed in the form of the letter C.
- Technique: Following positioning, the anesthetist cleans the back using an antiseptic solution. He or she may administer a local anesthetic to numb the skin prior to the insertion of the spinal needle.
- Anatomical Level: The anesthetic drug, which is usually Bupivacaine (a local anesthetic) is then injected into the subarachnoid space, usually between the lumbar vertebrae L3 and L4, through a long, thin needle, after ascertaining its correct position from the flow of the cerebrospinal fluid.The position after giving the block and the level of blockade achieved are subject to the drug volume and the surgery for which the block is given. The recovery from the effects of the blockade usually takes 6-8 hours.
Advantages of Spinal Anesthesia
- Relatively cheap
- Patient satisfaction
- Reduced risk of respiratory complications (which are more common with general anesthesia)
- Superior muscle relaxation

- Less bleeding
- Quick restoration of bowel function
- Reduced incidence of coagulation disorders following surgery
- Reduced post-operative stay
Disadvantages of Spinal Anesthesia
- The time required for the performance of the procedure varies depending on the anesthetist’s skill and competence.
- Potential risk of hypotension and meningitis due to improperly sterilized medical equipment.
- Postdural puncture headache (PDPH) and urinary retention are commonly observed post spinal block
- Risk of High/Total Spinal: This refers to blockade of the cardiac nerve fibers leadsto a severe drop in the heart rate and blood pressure. It is an emergency and needs to be managed by elective ventilation and resuscitation.
Contraindications of Spinal Anesthesia
- Absolute: Absolute contraindications include patients with abnormal bleeding and clotting parameters, local site infection, and patient refusal.
- Relative: Patients with severe fluid loss either by bleeding, vomiting, or diarrhea should be replaced with adequate fluids before being taken up for spinal anesthesia due to the risk of hypotension.
- Uncooperative patients, such as children, mentally challenged individuals, or patients with psychiatric disorders.
- Presence of neurological disease or raised intracranial pressure are relative contraindications for attempting a spinal block.
Spinal vs. Epidural vs. General Anesthesia: Which one is better?
Regional anesthesia offers a predictable level of blockade without manipulating the airway and ventilation of the patient. It offers a better intraoperative or post-operative analgesia as well. However, in patients requiring blockade at a level above the umbilicus and contraindications to regional blockade, general anesthesia is the safer choice.