Physiologists may have found a way to decrease the risk of hardening of the arteries that accompanies the long-term use of protease inhibitors, for effective treatment against HIV and AIDS.
Physiologists may have found a way to decrease the risk of hardening of the arteries that accompanies the long-term use of protease inhibitors, a class of drugs that has emerged as the most effective treatment against HIV and AIDS.
Writing in the American Journal of Physiology–Cell Physiology, researchers from the University of Kentucky found that when mice were given a nucleoside reverse transcriptase inhibitor (NRTI) and a protease inhibitor in combination, it prevented hardening of the arteries often associated with long-term use of protease inhibitors alone. The mice received ritonavir, a common protease inhibitor, in combination with d4T or didanosine, which are common NRTIs.“The combination prevented the negative cardiovascular effect, hardening of the arteries, of the protease inhibitors without reducing the effectiveness of the protease inhibitors on HIV,” said the study’s senior author, Eric J. Smart. “To our knowledge, these are the first data that indicate that nucleoside reverse transcriptase inhibitors can limit the atherogenic (tendency to form lipid deposits in the arteries) effects of ritonavir,” the authors wrote.
The study also found:
•Although protease inhibitors alone caused cholesterol to build up in mouse arteries, the increased cholesterol could not be detected in the blood. “This means that when doctors test for cholesterol on human patients who are using protease inhibitors, their cholesterol levels may look normal even when they are not,” Smart said. “In other words, the accumulation of cholesterol within the arteries is a silent problem.”
•Although Vitamin E, an antioxidant, has been shown to prevent the negative effects of protease inhibitors in vitro (in the test tube), the vitamin provided no benefit to the mice in this study.
Long-term side effects a concern
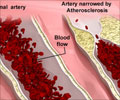
Protease inhibitors have been effective in prolonging the lives of people with AIDS, so much so that patients now survive long enough to develop side effects that are years in the making. One such side effect is atherosclerosis, the accumulation of cholesterol and foam cells in the arteries, causing the vessels to narrow and harden.
The problem occurs when cholesterol-laden macrophages get stuck in artery walls. Over time, they accumulate, block the arteries and can result in heart attacks. Because protease inhibitors prompt the CD36-rich macrophages to accumulate more cholesterol, the cholesterol and foam cells build faster and thus lead the arteries to harden more quickly, Smart explained.
The researchers examined macrophages isolated from mice receiving ritonavir, a protease inhibitor, and d4T and didanosine, both NRTIs. “NRTIs completely prevented the upregulation of CD36 and the development of atherosclerosis,” the authors wrote. Their results also suggest that the NRTIs prevented the increase in CD36 by decreasing protein kinase C, an enzyme that changes the function of proteins.
What’s more, NRTI reduced the negative effect of macrophages and cholesterol without reducing the effectiveness that ritonavir had against HIV. “So by giving both drugs at the same time, you get the positive effects of the protease inhibitors without the negative effect of hardening of the arteries,” Smart concluded.
The researchers are now beginning a short-term study with healthy human volunteers to see if the protease inhibitor/NRTI drug combination will help control the production of CD36 in humans as well, Smart said.
“We’ll try to find out if the NRTI regimen can keep the CD-36 protein in check in the non-infected volunteers,” Smart said. If the drug combination works, the researchers will move to further clinical trials.
Source-Newswise
SRM
 MEDINDIA
MEDINDIA
 Email
Email