Human papilloma virus vaccination programs have substantially reduced the number of infections and precancerous cervical lesions caused by the virus.
‘Women of reproductive age are advised to take HPV vaccination as there is significant reduction in the infections that cause cervical cancer and precancerous lesions. It could ultimately lead to the elimination of cervical cancer as a public health problem.’
Read More..




Infections caused by HPV are among the most common sexually transmitted diseases. Certain forms of the virus can lead to anogenital warts while others cause lesions that can develop into cancer of the mouth, throat, vagina, vulva, anus, or penis, and particularly the cervix. "HPV is found in almost 100% of cervical cancer cases," states lead author Mélanie Drolet. Read More..
The research team headed by Université Laval's Faculty of Medicine Professor Marc Brisson performed a meta-analysis of 65 studies in 14 different countries that have set up HPV vaccine programs in the last ten years. With data on 60 million people, the researchers compared the frequency of HPV infections, anogenital warts, and precancerous cervical lesions before and after the programs were launched.
Their analysis shows that infections dropped by 83% among girls aged 13 to 19 and 66% among women aged 20 to 24. For anogenital warts, the drop was 67% among 15- to 19-year-old girls, 54% for women aged 20 to 24, and 31% for those aged 25 to 29. Precancerous cervical lesions also dropped by 51% among teens aged 15 to 19 and 31% among women aged 20 to 24.
Vaccination of young women is also producing herd protection for young men. Anogenital warts among males have dropped 48% for those 15 to 19 and 32% for those aged 20 to 24.
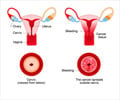
Cervical cancer currently affects 1 woman in 150 in Canada, and the 5-year mortality rate is about 25%. "HPV vaccination is still too recent to directly measure its effects on cervical cancer as it can take decades to develop," explains Mélanie Drolet. "However, our analyses show that vaccination is producing substantial reductions in the infections that cause cervical cancer and precancerous lesions. These reductions are a first sign that vaccination could eventually lead to the elimination of cervical cancer as a public health problem. We are now trying to determine when elimination could be achieved and which vaccination and screening programs could help us achieve it faster."
Advertisement
Source-Eurekalert