At the University of Cambridge, researchers have discovered that a single mutation in a leukemia-associated gene reduces the ability of blood stem cells to make more blood stem cells, but leaves their progeny daughter cells unaffected.
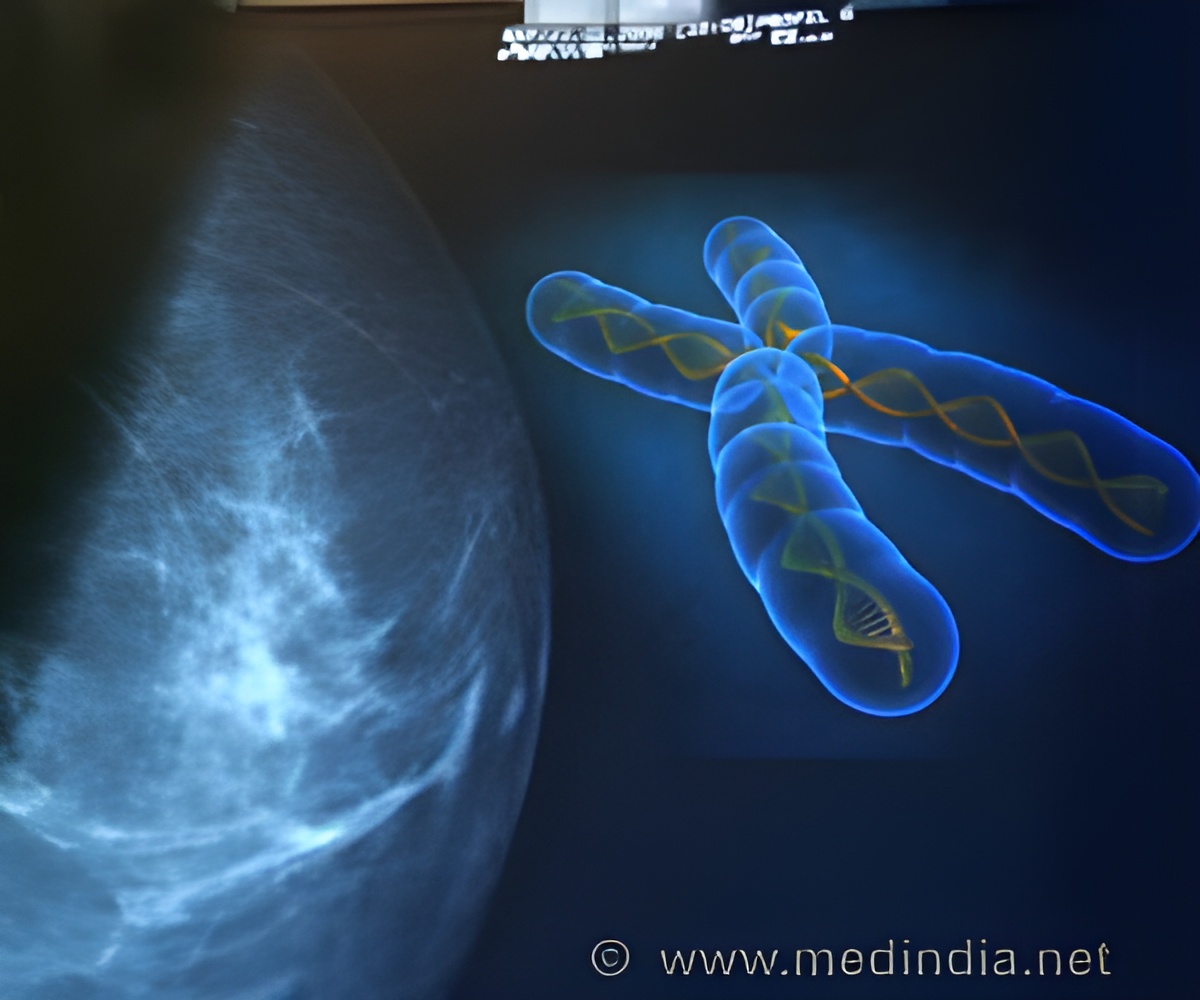
Published this week in PLOS Biology, the study by Professor Tony Green and his team at the Cambridge Institute for Medical Research is the first to isolate highly purified single stem cells and study their individual responses to a mutation that can predispose individuals to a human malignancy. This mutation is in a gene called JAK2, which is present in most patients with myeloproliferative neoplasms (MPNs)—a group of bone marrow diseases that are characterized by the over-production of mature blood cells and by an increased risk of developing leukemia.
Using a unique mathematical modeling approach, carried out in collaboration with Professor Ben Simons at the Cavendish Laboratory in Cambridge, in combination with experiments on single mouse stem cells, the researchers identified a distinct cellular mechanism that operates in stem cells but not in their daughter cells.
"This study is an excellent example of an inter-disciplinary collaboration pushing the field forward," says lead author Dr David Kent. "Combining mathematical modeling with a large number of single stem cell assays allowed us to predict which cells lose their ability to expand. We were able to reinforce this prediction by testing the daughter cells of single stem cell divisions separately and showing that mutant stem cells more often undergo symmetric division to give rise to two non-stem cells."
Characterizing the mechanisms that link JAK2 mutations with this pattern of stem cell division—a pattern that eventually leads to the development of MPNs—will inform our understanding of the earliest stages of tumor establishment and of the competition between tumor stem cells, say the authors. The next step, currently underway at the Cambridge Institute for Medical Research, is to understand the effect that acquiring additional mutations has on blood stem cells, as these are thought to drive the expansion of blood progenitor cells, leading to the eventual transformation to leukemia that occurs in patients with MPNs.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email









