The non-alcohol fatty liver disease Research Center was launched to better understand the disease and develop treatments where none currently exist.
TOP INSIGHT
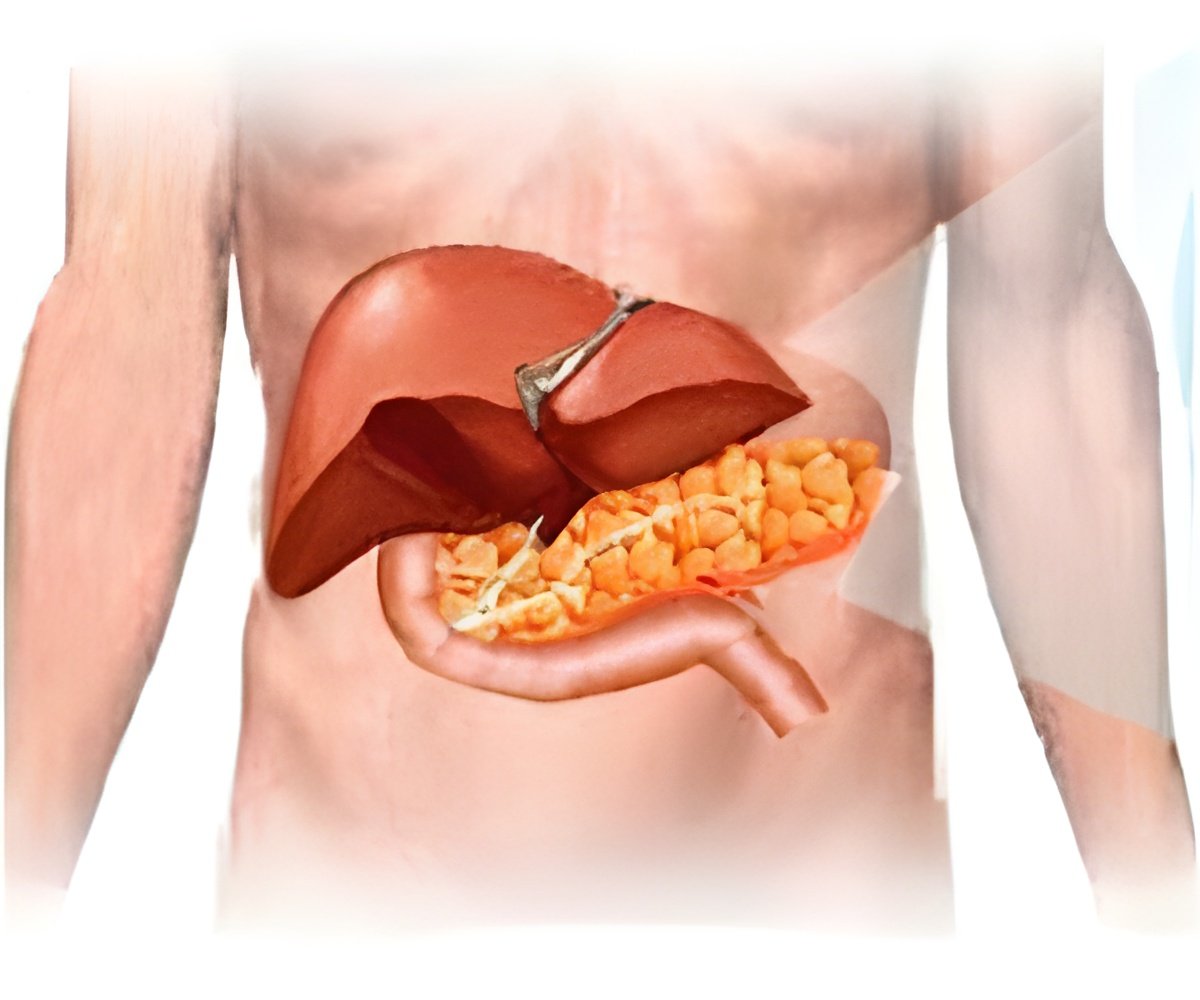
Non-Alcohol Fatty Liver Disease can progress to nonalcoholic steatohepatitis, a more extreme form of the disease, which can, in turn, result in cirrhosis or liver cancer.
"In pharmacology, molecular medicine, physician training, clinical trial design and drug development, scientists and researchers here have been working on NALFD and related diseases for a long time. But this is a major step. It creates a single entity able to address every aspect of a global disease that didn't even exist 35 years ago."
NAFLD occurs when fat accumulates in liver cells due to causes other than excessive alcohol use. The precise cause is not known, but diet and genetics play substantial roles. Up to 50 percent of obese people are believed to have NAFLD. The condition is particularly prevalent among Hispanics and Asians.
NAFLD can progress to nonalcoholic steatohepatitis (NASH), a more extreme form of the disease, which can, in turn, result in cirrhosis or liver cancer. In most cases, adverse effects are not noticeable until the disease is well-advanced. NAFLD is closely linked to diabetes.
"In 2000, just 2 percent of liver transplants were caused by the eventual effects of NAFLD," said Loomba. "In 2011, it was the third leading indicator for transplant and may soon be the leading indication for liver transplant."
To that end, researchers at UC San Diego have already made progress, developing a diagnostic tool using magnetic resonance imaging that avoids the current requirement of a liver biopsy for assessment of treatment response in early phase clinical trials. "This is a key advance because it means you can conduct clinical trials with a tool that is effective but non-invasive and get an early signal of efficacy."
Loomba and colleagues have also designed and conducted several ground-breaking clinical trials for NAFLD and NASH. The creation of the center provides a one-stop shop for all areas of investigation in NASH. The newly created NAFLD research center, said Loomba, would attract collaborations with biotechnology industry as well as to pharmaceutical companies that have a biomarker development program or are looking for expertise in innovative clinical trial design.
"This center will act as an epicenter for NASH clinical drug development and as a catalyst in biomarker discovery, validation and their application in clinical practice," said David Brenner, MD, vice chancellor for health sciences, dean of the School of Medicine and professor of medicine in the Division of Gastroenterology.
The NAFLD Research Center brings together multiple specialties and specialists at UC San Diego School of Medicine and elsewhere:
Source-Medindia
 MEDINDIA
MEDINDIA
 Email
Email