Researchers identify certain lifestyle factors that make it more likely for a woman to enjoy a healthy pregnancy.
Although further work is needed to determine whether these associations have causal importance, this study implies that targeted interventions that encourage women to make healthy choices before and during pregnancy "may increase the likelihood of normal pregnancy outcomes," write the authors.
Previous research has focused on the association between risk factors and subsequent adverse pregnancy outcomes, but little is known about factors associated with subsequent healthy pregnancies.
Researchers from the UK, Ireland and New Zealand therefore carried out a study to identify factors at 15-20 weeks' gestation associated with a subsequent uncomplicated pregnancy. Their aim was to highlight those factors amenable to change before pregnancy, thereby informing decisions about interventions that could increase the likelihood of a normal outcome.
A total of 5,628 healthy women with singleton births (and no previous pregnancies) were recruited to the Screening for Pregnancy Endpoints study between November 2004 and August 2008 (3196 from Australia and New Zealand and 2432 from the UK and Ireland).
The primary outcome was uncomplicated pregnancy defined as a "normotensive pregnancy, delivered at more than 37 weeks resulting in a live born baby who was not small for gestational age and did not have any other significant pregnancy complications".
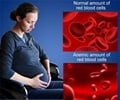
The most common reasons for a complicated pregnancy in the mother were gestational hypertension (8%) and pre-eclampsia (5%) and in babies was being small for gestational age (11%) and spontaneous preterm birth (4%).
Factors amenable to improvement that increased the likelihood of an uncomplicated pregnancy (that is, were beneficial) were high fruit intake in the month before pregnancy and being in paid employment 15 weeks into pregnancy.
Detrimental factors that could not be altered were being in a lower socio-economic group, high blood pressure before pregnancy while taking oral contraceptive pills, family history of high blood pressure in pregnancy and bleeding during pregnancy.
Lifestyle recommendations already exist for non-hypertensive people to optimise their blood pressure through physical exercise, weight reduction, limiting salt intake and alcohol consumption, and consuming a healthy diet, explain the authors. "Our study suggests that adoption of these choices seems to be beneficial in determining uncomplicated pregnancy."
For example, a 5 mm Hg reduction of maternal systolic blood pressure would increase the proportion of uncomplicated pregnancies by 3% equating to 24,674 more UK women having an uncomplicated pregnancy. They say, however, that this requires demonstration in a randomised controlled trial.
They point to a "growing interest" in promotion of health and normality, rather than a focus on adverse outcomes and say that, if confirmed, "this study should inform development of interventions to increase normal pregnancy outcomes."
In an accompanying editorial, Professor Knight from the Nuffield Department of Public Health says the most important next step is to focus on "normality rather than abnormality", to guide population interventions. She says that the study provides useful information for women, clinicians and policy-makers but the challenge that remains is identifying the interventions needed to achieve the desired changes in risk.
Knight adds that consideration has to be given to interventions "designed to improve pregnancy outcomes with more general population programmes" as well as further research "to assess factors associated with uncomplicated pregnancy" in women with underlying medical conditions.
Source-Eurekalert
 MEDINDIA
MEDINDIA




 Email
Email