A new research may have unearthed why women get migraines more often then men. For every man with a migraine, three women are struck by the severe headaches that often come with
A new research may have unearthed why women get migraines more often then men.
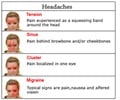
For every man with a migraine, three women are struck by the severe headaches that often come with nausea, sensitivity to light and sound, and aura.The research, by boffins at University of California Los Angeles (UCLA), has now suggested that this happens because women have a faster trigger than men for activating waves of brain activity thought to underlie migraines.
As a part of the study, lead researchers Dr. Andrew Charles, director of the Headache Research and Treatment Program in the UCLA Department of Neurology; Dr. Kevin C. Brennan, a clinical and research fellow in Charles' lab; and colleagues used a mouse model to discover a big difference between males and females with regard to a phenomenon called cortical spreading depression (CSD), which is thought to be a chief culprit in causing migraines.
Dr. Brennan, working in Dr. Charles' lab, used imaging techniques to visualize the initiation and spread of CSD in anaesthetized male and female mice.
Female mice showed a significantly lower threshold for CSD when compared with males. In other words, it was much easier to evoke the waves of brain activity believed to underlie migraine in females than it was in males.
'The results were very clear. The strength of the stimulus required to trigger CSD in males was up to two or three times higher than that required to trigger the response in females,' said Charles.
The researchers also noted that while it is known that migraines in females fluctuate with the menstrual cycle and are more frequent during the menstrual period, the study results suggest that this is independent of a specific phase of the cycle.
'Yet we still found a consistent difference in the CSD threshold between males and females. Our results suggest that the female brain has an intrinsic excitability that predisposes them to migraine that may not be simply linked to a specific phase of the menstrual cycle.'
These results are exciting, Charles said, because they may represent a model for understanding the mechanisms underlying the increased prevalence of migraine in women.
18 to 25 percent of women suffer from migraines, making it one of the most common disabling conditions faced by women around the globe.
In addition, they add to growing evidence that CSD is a key target for the development of new migraine treatments.
Funded by the National Institutes of Health, the study appears in the Annals of Neurology.
In a separate study, the researchers identified what they hope will eventually be a new treatment option for migraine. They found that a medication called memantine (brand name Namenda), which is currently approved for the treatment of Alzheimer's disease, inhibits CSD and appears to be a highly effective treatment for some patients with frequent migraine.
In the second study, 54 patients who were treated with memantine for at least two months were asked to fill out a survey describing their experience with the medication. The majority, 36, reported a substantial reduction in estimated headache frequency. These were all patients who had previously tried other treatments without success.
This study is to be published in the September issue of the Journal of Headache and Pain.
Source-ANI
LIN/J
 MEDINDIA
MEDINDIA
 Email
Email