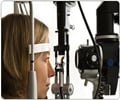
In a new study, Mayo Clinic researchers have identified that a sleep disorder called obstructive sleep apnea (OSA) may lead to various eye diseases.
In a new study, Mayo Clinic researchers have identified that a sleep disorder called obstructive sleep apnea (OSA) may lead to various eye diseases.
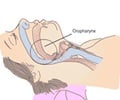
OSA is a potentially serious sleep disorder in which breathing repeatedly stops and starts during sleep and it occurs when throat muscles relax and block the airway.A large number of studies have identified OSA as an independent risk factor for the development of several medical conditions, like high blood pressure, which are related to impairments or alterations in a person's vascular (circulatory) system.
And eyes, with their own complex and sensitive vascular system, can sometimes signal and be affected by systemic vascular problems.
"Given the vascular consequences of OSA, it is not surprising that ophthalmologic manifestations exist," explained lead author, E. Andrew Waller, M.D., a Mayo Clinic pulmonologist and sleep specialist.
For the study, the researchers conducted a literature search focused on sleep disorders and eye disease.
In their study, the scientists have listed a variety of ophthalmologic conditions associated with obstructive sleep apnea, some of which are as follows:
Glaucoma: This condition is the second most common cause of blindness and the most common cause of irreversible blindness. OSA is linked to two forms of this disease, primary open-angle glaucoma (POAG) and normal-tension glaucoma (NTG). The severity of glaucoma appears to correlate with the number and duration of apnea episodes in patients with OSA.
Papilledema: People with OSA may have a higher incidence of papilledema, swelling of the optic nerve in both eyes. Papilledema typically occurs due to increased pressure within the skull and can lead to progressively worsening vision and, in some cases, blindness.
Waller said that the knowledge of the links between these eye conditions and OSA may pave the way for early diagnosis and appropriate treatment.
"Our understanding of the mechanisms that link these disorders is minimal. However, the recognition of these associations is important for primary care physicians, ophthalmologists, and sleep physicians. For patients with OSA, a routine eye examination to evaluate for early signs of glaucoma, particularly in the setting of visual loss or change, should be recommended. Patients with ophthalmologic diseases known to be associated with sleep apnea should be screened clinically for sleep apnea and referred to a sleep center if signs or symptoms are present," said Waller.
The study is published in the latest issue of Mayo Clinic Proceedings.
Source-ANI
SRM
 MEDINDIA
MEDINDIA



 Email
Email