Using Continuous positive airway pressure, a therapy for sleep apnea, improved insulin sensitivity and reduced risk of heart disease in diabetics.
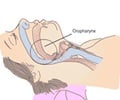
Continuous positive airway pressure (CPAP), the device used to treat obstructive sleep apnea (OSA) appears to improve glycemic control in diabetics, according to research published in the American Thoracic Society's
American Journal of Respiratory and Critical Care Medicine. //
Francisco Garcia-Rio, MD, PhD, professor of medicine at Autonoma University of Madrid and senior study author, said the research advanced understanding of the biological relationship between two major public health problems, which epidemiological studies have indicated are related.
TOP INSIGHT
The levels of inflammatory molecules IL-1, IL-6 were reduced and levels of adiponectin, an important glucose regulator improved, after the use of Continuous positive airway pressure in diabetics.
"OSA is a public health problem of the first order, due to its high prevalence and marked morbidity and mortality, having been linked to traffic accidents, cardiovascular complications and, more recently, neoplastic diseases," he said. "Diabetes mellitus is a global epidemic. There are currently 382 million diabetics worldwide, a figure which is estimated to reach 592 million in 2035."
Dr. Garcia-Rio and his colleagues studied results from 50 patients with both OSA and sub-optimally controlled type 2 diabetes, who were assigned to CPAP intervention or control. Participants, who ranged in age from 18 to 80, did not change diabetes medications during the trial unless medically necessary, nor were they expected to change their diets or level of physical activity.
In addition to measuring glucose control, researchers measured changes in insulin sensitivity and resistance, inflammatory proteins and other biomarkers that may be associated with type 2 diabetes glycemic control. Researchers found that those using CPAP showed a statistically significant:
- Decrease in glycated hemoglobin (HbA1c) levels at 6 months. (The decrease at 3 months was not statistically significant.)
- Improvement in insulin sensitivity at 3 and 6 months.
- Decrease in insulin resistance at 6 months.
Researchers also found CPAP participants experienced lower levels of the inflammatory molecules IL-1; and IL-6 and higher levels of the hormone adiponectin, an important glucose regulator.
Authors noted that previous studies reported a 1 percent decrease in HbA1c levels was associated with 15-20 percent decrease in major cardiovascular disease events and a 37 percent decrease in microvascular complications from diabetes. If the association proves true, the authors said the 0.4 percent reduction in HbA1c in their study might translate into a 6-8 percent decrease in cardiovascular disease risk and a 15 percent reduction in microvascular complication risk. They added that their study also found those in the CPAP group experienced a significant reduction in LDL cholesterol, an established risk factor for cardiovascular disease.
Dr. Garcia-Rio said study findings suggest that "early identification of OSA in patients with type 2 diabetes, and assessment for metabolic abnormalities in those with OSA could reduce the cardiovascular disease risk of patients with these chronic diseases."
Researchers believe results are generalizable, given that patients included in the study were referred from diabetes units or primary care physicians, reflecting standard clinical practice. Study limitations include small sample size, lack of a placebo arm and medication changes that were necessary for some patients during the trial.
Source-Eurekalert

 MEDINDIA
MEDINDIA



 Email
Email