Along with several other factors, both severely restricted and excessive fetal growth may be associated with stillbirth, reveals a study by US researchers.
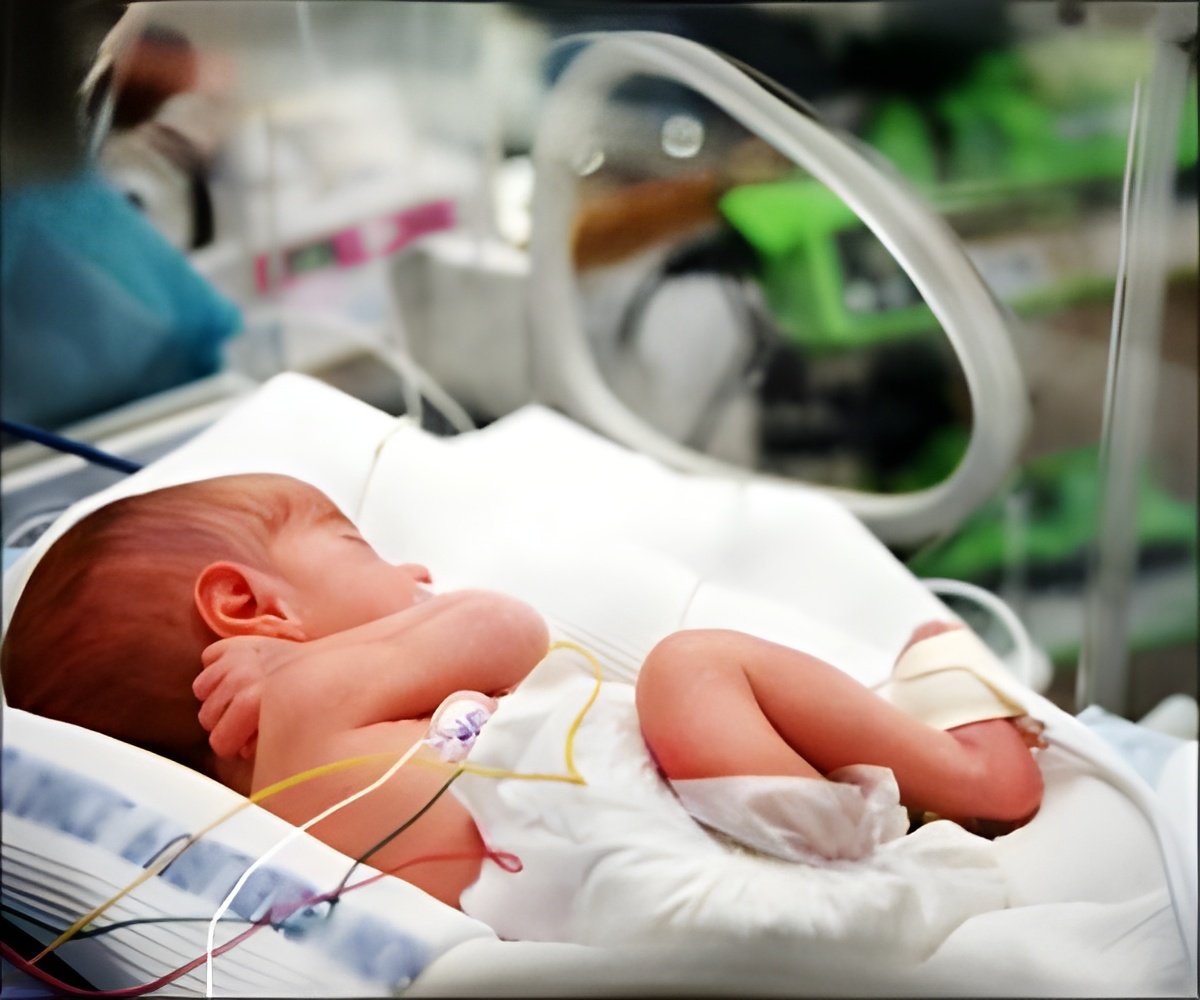
Using this approach the authors investigated all the stillbirths, and a sample of live births, which occurred over 2 and a half years at 59 hospitals in five US regions.
The authors found that overall, abnormal fetal growth was identified in 25% of stillbirths using population norms and in above 50% of stillbirths using ultrasound or individualized norms: Small for Gestational Age (SGA: the bottom 10% of the population weight for gestational age) was associated with a 3- to 4-fold increased risk of stillbirth compared to having a fetus with "appropriate" weight for gestational age based on all three norms. Large for Gestational Age (LGA: the top 10% of the population weight for gestational age) was associated with an increased risk of stillbirth based on the ultrasound and individualized norms but not the population norms. Being more severely SGA or LGA (below the 5th percentile or above the 95th percentile) was associated with an increased risk of stillbirth.
Although the accuracy of these findings is likely to be affected by aspects of the study design, these findings suggest that, contrary to current practices, strategies designed to prevent stillbirth should focus on identifying both severely SGA and severely LGA fetuses.
The authors say: "When accounting for time of death and using norms developed in normal pregnancies, both SGA and LGA birth weights were associated with stillbirth in our study.
They continue: "The association is mainly related to severe SGA and LGA pregnancies, with birth weights either below the 5th or above the 95th percentile. Thus, classifying 10% of pregnancies as abnormally grown has the potential to identify 44%-46% of future stillbirths."
 MEDINDIA
MEDINDIA

 Email
Email