Researchers have found that the detection of atrial fibrillation (irregular heart rhythm), a major risk factor for stroke, can be improved by actively screening elderly people.
Researchers have found that the detection of atrial fibrillation (irregular heart rhythm), a major risk factor for stroke, can be improved by actively screening elderly people.
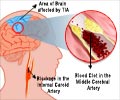
As people grow old, the prevalence of atrial fibrillation rises from about one per cent in the whole population to about five per cent in people aged over 65. A simple low cost test called electrocardiography can help diagnose it, and the risk of serious problems like stroke can be dramatically reduced by treatment.There are two types of screening for atrial fibrillation- opportunistic and systematic (total population) screening. In the former, a healthcare professional takes a patient's pulse during a consultation and, if the pulse is irregular, electrocardiography is performed to confirm the diagnosis. Whereas in systematic screening, the whole target population is invited for screening by electrocardiography.
With a view to testing whether screening was more effective than routine care in detecting atrial fibrillation in the community, the researchers compared opportunistic with total population screening. They identified 14,802 patients aged 65 or over from 50 general practices (split into 25 intervention and 25 control practices) in England.
Participants in intervention practices were randomly allocated to systematic screening or opportunistic screening. Screening took place over 12 months in each practice from October 2001 to February 2003. No active screening took place for participants in control practices.
The researchers noted that screening practices identified substantially more cases of atrial fibrillation than control practices, and that both systematic and opportunistic screening detected similar numbers of new cases.
The two screening processes did not raise anxiety and were acceptable to patients.
Advertisement
They concluded that the more labour intensive, costly, and intrusive approach with systematic screening could not be justified because the detection rates were identical for the two methods.
Advertisement
Source-ANI
SRM/J