Researchers began by injecting all candidate genes into the human fibroblasts, then systematically removed each one to see which were necessary for reprogramming and which were dispensable.
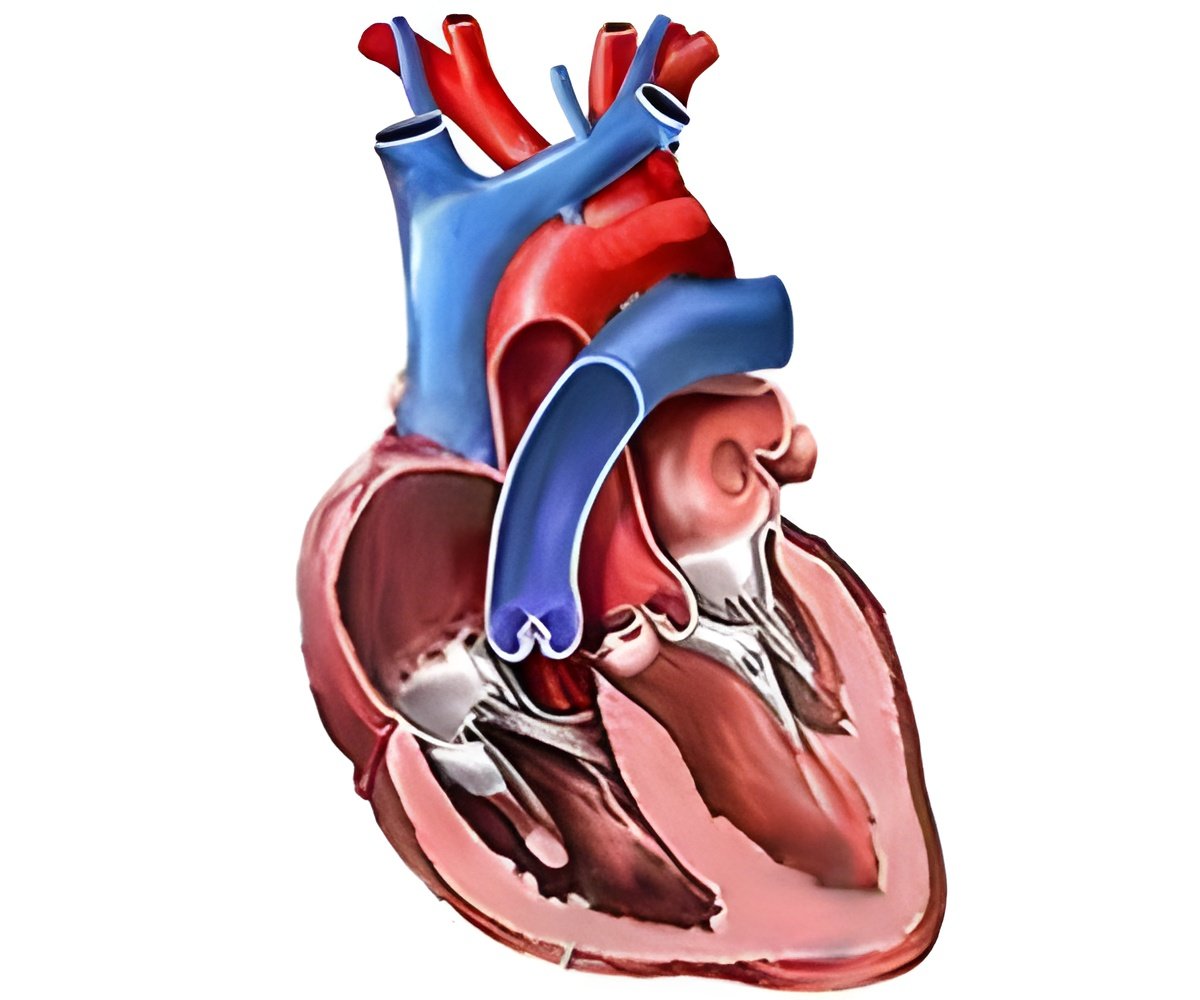
"While almost all the cells in our study exhibited at least a partial transformation, about 20% of them were capable of transmitting electrical signals—a key feature of beating heart cells," said Dr. Fu. "Clearly, there are some yet-to-be-determined barriers preventing a more complete transformation for many of the cells. For example, success rates might be improved by transforming the fibroblasts within living hearts rather than in a dish—something we also observed during our initial experiments in mice."
The immediate next steps are to test the five-gene cocktail in hearts of larger mammals, such as pigs. Eventually, the team hopes that a combination of small, drug-like molecules could be developed to replace the cocktail, offering a safer and easier method of delivery.
"With more than five million heart attack survivors in the United States, who have hearts that are no longer able to beat at full capacity, our findings—along with recently published findings from our colleagues—come at a critical time," added Dr. Srivastava. "We've now laid a solid foundation for developing a way to reverse the damage—something previously thought impossible—and changing the way that doctors may treat heart attacks in the future."
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email