Stimulation of the brain has become a popular science with the advent of non-surgical modalities and researchers must work to ensure systematic methods for consistent results in the study of stroke rehabilitation.
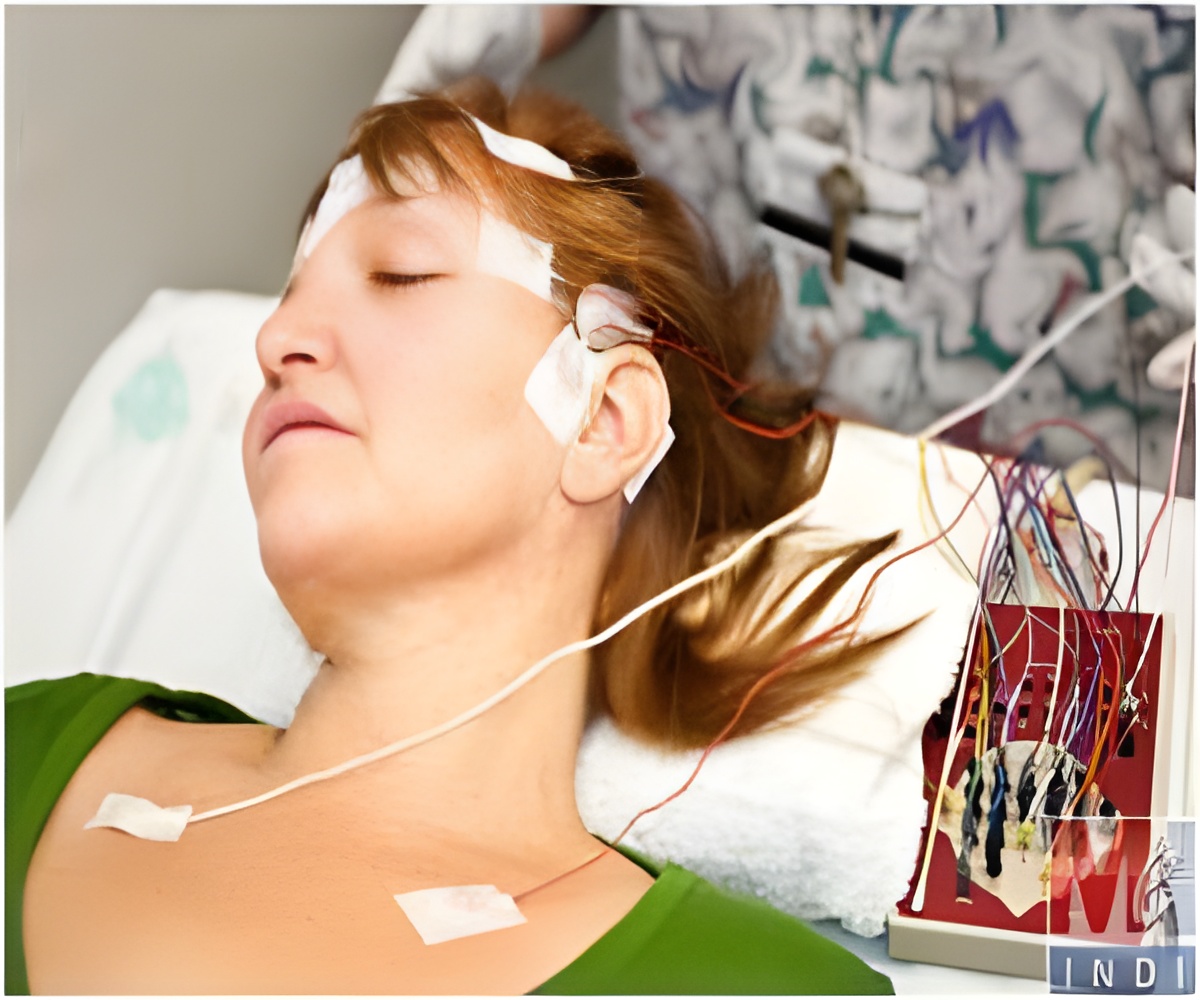
"Before therapeutic potential of brain stimulation is missed amidst the enthusiasm for its ability to augment brain activity, it is urgent to systematically understand whom stimulation of the brain may benefit, how, and why," said study author Dr. Ela Plow from the Biomedical Engineering, Lerner Research Instt. at the Cleveland Clinic Foundation. "Addressing the challenge first in stroke is critical, not just because stroke is the leading cause of long-term adult disability, but also because the field was one of the first to report on therapeutic potential of brain stimulation, but unfortunately the first to witness some of its most noted conflicts as well."
Using a conceptual model, researchers Ela B. Plow, David A. Cunningham, Nicole Varnerin, and Andre Machado suggest expanding the scope of stimulation to include other substrates, such as premotor and supplementary motor cortices that are more likely to survive damage in humans, offer their independent output, and collaborate with areas in the intact hemisphere to recruit their cooperation towards recovery as well. Rather than propose that these substrates could serve as the be-all-end-all of plasticity, the researchers suggest that their role may be more meaningful in those with greater damage and do not discount the possibility of success for other substrates such as cerebellum, striatum, parietal cortices etc.
Dr. Plow continued, "Conflicting evidence in stroke has dampened the enthusiasm for brain stimulation witnessed across several hundred early studies in the last decade, limiting the potential of clinical outpatient or even inpatient delivery in the immediate future. Before starting another clinical trial and waiting to see if by chance the new study shows positive effects, we suggest re-evaluating and shifting perspective."
The researchers outline the journey of stimulation in stroke rehabilitation from trials with homogeneous animal models, to early clinical studies where patients with greater sparing of motor cortices and spared output responded exceptionally well to stimulation of their residual cortex, to larger clinical trials that enrolled the more impaired such as those with greater damage to cortices, in which stimulation of motor cortices failed to uniformly augment outcomes of recovery.
With such differences among trial groups, the researchers found that a great discordance between early and later, larger clinical studies resulted. Dr. Plow commented, "By following a one-size-fits-all approach, we risk relying only on pure chance."
"Our intent here is to create a shift in perspective that forces us to broaden scope of stimulation from affecting a single target and a single mechanism to imagining how and what may remain to assume the potential for recovery in humans," Dr. Plow continued. "We even suggest that targets may not even need to be uniform across all, because it may leave outcomes of trials to pure chance. Instead, we believe systematically exploring substrates and defining successes and failures of each would truly create personalized, not popular science."
 MEDINDIA
MEDINDIA


 Email
Email