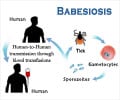
The cell signalling pathway used by parasites that cause malaria and toxoplasmosis to escape from and destroy their host cells and infect new cells has been identified.
When the Plasmodium falciparum and Toxoplasma gondii parasites invade a host cell, they take up residence inside a "parasitophorous vacuole" (PV), growing and replicating themselves for about 48 hours.
Then they burst out of the PV, completely destroying and dissolving the protein-based cytoskeleton of their host, freeing themselves to seek out and infect new host cells.
Doron Greenbaum's previous work showed that both P. falciparum and T. gondii hijack the calcium-regulated enzyme calpain from host cells and use it to break down host cytoskeleton.
The current study by researchers from the Perelman School of Medicine, University of Pennsylvania and Johns Hopkins University took the next step of identifying which host signalling pathway was involved, with the aim of derailing the parasite's escape route, trapping it inside the host cell and preventing it from spreading infection.
"We found an entire signaling pathway in the human host cell that the parasite engages, starting from a G-protein-coupled receptor, that the parasite uses to dismantle the cytoskeleton of the host cell, causing it to collapse," Greenbaum, study leader from the Pharmacology at Penn, said.
Independent of calpain, the researchers also found that host PKC played an important role in the loss of protein adducin from the host cytoskeleton, contributing greatly to its collapse.
"It's a human enzyme [PKC] that we're targeting, and by inhibiting it we've basically blocked the parasites from getting out. They're trapped and die within the host cells," Greenbaum said.
A key advantage of such an approach, explains Greenbaum, is that "targeting a host protein will engender less resistance because the parasite has no genetic control over the host."
One of the inhibitors tested was a new orally available agent called sotrastaurin, a PKC inhibitor.
This drug has already passed Phase I trials and is currently undergoing Phase II trials for various indications. In the mouse studies, sotrastaurin administration also resulted in a significant decrease in parasitemia and markedly increased survival rates against Plasmodium berghei ANKA, thus showing great potential as an oral antimalarial.
"We've piggybacked this line of research onto a drug class that's already vetted," says Greenbaum.
"We're quite excited about that. We've found a compound that's already been used in trials in humans and is deemed safe," he said.
Greenbaum and his team are hopeful that after more extensive animal testing, the next step could be human trials of sotrastaurin against malaria. This compound, or similar PKC inhibitors, could provide a multipronged weapon against malaria and other parasitic disease.
"This approach could be used as both a prophylactic and a treatment," Greenbaum said.
"We have some indication that it could also used to block transmission," he added.
The study has been published in Cell, Host and Microbe.
Source-ANI
 MEDINDIA
MEDINDIA



 Email
Email