Researchers are reporting that studies on lab animals have shown early success in a type of gene therapy that may prevent the spread of pandemic flu.
The research is still in its initial stages, but could offer a new tool against influenza infections which kill 500,000 people globally each year, scientists said.
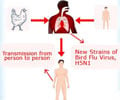
A single dose appeared to protect mice for as long as nine months against a range of flu strains, including three strains of H5N1, a deadly bird flu, and and two strains of H1N1, known widely as the "swine flu" that emerged in 2009.
Typically, influenza viruses evolve so rapidly that a new vaccine is created each year, offering only limited protection against the flu which can be lethal particularly in the elderly and those with weak immune systems.
The research published in the journal Science Translational Medicine did not experiment with the latest form of bird flu to emerge from China, H7N9, which has killed 37 of the 132 people infected since March.
According to a separate study in The Lancet on Tuesday, some H7N9 bird flu patients have already been found to be resistant existing antivirals, likely as a result of treatment with Tamiflu.
"Further development of this approach for pandemic flu has taken on more urgency in light of the spreading infection in China of the lethal bird strain of H7N9 virus in humans."
The method uses adeno-associated virus vectors based on a primate virus, AAV9, to deliver broadly neutralizing antibodies to a section of the flu virus that is not believed to evolve as rapidly as other parts.
If the technique can be proven to work in people, its benefits would include speed of use against a pandemic -- which usually does not allow enough time to develop an effective treatment -- and a non-invasive, low cost application.
"Overall, the information is pretty useful," said Suresh Mittal, a professor of comparative pathobiology in Purdue's College of Veterinary Medicine, who was not involved in the research.
He said more needs to be done to determine the optimal dosage in humans, to find out how long the protective effects may last and if influenza can find a way to outsmart even a broadly neutralizing antibody.
"But as usual, once the new information comes in there will be a lot of other work that needs to be done," Mittal told AFP.
Clinical trials in humans to evaluate the use of adeno-associated virus vectors as gene delivery agents in cancer therapy are already under way.
Source-AFP
 MEDINDIA
MEDINDIA

 Email
Email




