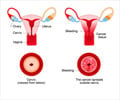
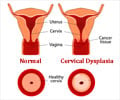
Dr Neeta Singh, Professor and Head of Department of Biochemistry, All India Institute of Medical Sciences (AIIMS), said 528,000 cases of cervical cancer occur globally, out of which 132,082 are in India. 273,500 women die of cervical cancer globally every year, out of which 74,118 deaths occurred in India.
Dr Smita Joshi, Associate Professor, Department of Preventive Oncology, Hirabai Cowasji Jehangir Medical Research Institute, Pune, said that almost 85% of cervical cancer deaths occur in countries where there is a lack of population-based cervical cancer screening programmes for all eligible 30-50 years old women. Almost 200 women died every day due to cervical cancer in India, which is essentially preventable.
Dr Neeta Singh said that majority of the people who have HPV infection will clear the virus in 1-2 years and do not develop cervical cancer. Human body’s immune system usually eliminates the HPV infection on its own. Cervical HPV infection usually becomes undetectable within 2 years in 90% of women. She cautioned that we need to watch out for women where HPV infection persists and can cause a variety of serious health problems.
Health problems that can be caused by HPV include: genital warts; cervical cancer (cancer on a woman's cervix); and cancers of the vulva, vagina, penis, or anus; and a type of head and neck cancer called oropharyngeal cancer.
Dr Singh added that lifetime risk to ever contract HPV infection is 80% so it is better to get screened regularly. She said that even if the person has been vaccinated it is recommended to go for regular screening as there are a number of HPV strains.
Advertisement
NOT JUST FEMALES, MALES TOO AT RISK OF HPV CANCERS
Advertisement
In a study on anal HPV infection in Indian HIV positive men who have sex with men (MSM) at two sites in India, Christian Medical College (CMC) Vellore and Humsafar Trust Mumbai, rates had set the alarm bells ringing. 90% HPV infection was reported from CMC Vellore site and 95% HPV infection among study participants at Humsafar Trust Mumbai. In CMC Vellore those HIV positive MSM who participated in the study were more likely to be married and elder than the cohort in Mumbai (which was less likely to be married and younger in age).
VACCINE EXISTS FOR SOME STRAINS OF HPV
Dr Palefsky said that quadrivalent vaccine is effective in preventing HPV infection and cancers. It is effective against the following HPV types: 6, 11, 16 and 18 among others.
In USA, this vaccine is approved for routine use to prevent: genital warts; vulvar, vaginal, cervical and anal cancers in girls and women aged 9-26 years; and gential warts and anal cancer in boys and men aged 9-21 years and in immunocompromised or HIV positive men who have sex with men (MSM) aged 9-26 years.
Dr Palefsky argued that current vaccines may reduce cervical cancer by up to 70%, and newer vaccines may further reduce rates by more than 90%. HPV vaccines have an excellent safety record with no evidence of any serious adverse events attributed to it, said Dr Palefsky.
Dr Palefsky recommended rolling out HPV vaccination in India. School based approach is good as trying to vaccinate young girls outside of schools will be extremely challenging. In USA, one-third of young girls get vaccinated in schools. School-based roll-out may help to reach out to young girls and boys to prevent them from HPV related cancers and other complications later in life.
ARE WE DOING CERVICAL CANCER SCREENING IN A MAJOR WAY?
Dr Balaiah Donta, who is a senior scientist at National Institute for Research in Reproductive Health (NIRRH), an Indian Council of Medical Research (ICMR) institute, and also one of the organizing secretaries of this conference, said: a very small percentage of women undergo pap smear screening due to lack of awareness and due to deep rooted patriarchy, as men continue to play a key role in women’s health seeking behaviour. Dr Smita Joshi added that according to a study, less than 10% women in India access cervical cancer prevention services. Unless we improve the cervical cancer screening in our country, its rates are unlikely to decline in our country.
Dr Palefsky argued that HPV vaccination is thus the best approach to prevention of HPV related cancers in India because current approaches to cervical cancer control in India are not working well enough. HPV vaccines are safe and immunogenic in HIV infected men and women too.
In a study done by Dr Donta in maternity homes in Mumbai, only 4.5% of 18-49 years aged wives had heard of pap smear screening, but none of their male partners had heard of it. Likewise although 31.9% of 30-39 years aged wives had heard of cervical cancer only 4.5% of husbands had ever heard of it.
Dr Donta said that lower levels of awareness on cervical cancer and pap smear screening is an important barrier to cancer control. Among this cohort of couples, 32.3% women had HPV infection, 27% had bacterial vaginosis (BV), 8.3% had monilia fungus infection, 7.9% had chlamydia, and 0.5% had trichomonas vaginalis.
DOUBLE TROUBLE: HPV and HIV CO-INFECTION
Dr Smita Joshi said to Citizen News Service (CNS) that not only those who are HPV infected have increased risk of HIV acquisition but women living with HIV too have an increased risk of HPV infection of multiple strains, and it is more likely that HPV infection may persist for long leading to cervical intraepithelial neoplasia (CIN) and cervical cancer too. Studies show that women living with HIV have 2-22% increased risk of cervical cancer.
Cancer registry data in the developed counties have shown a rise in cervical cancer incidence in HIV infected women on antiretroviral therapy (ART). Dr Joshi recommended cervical cancer screening every 5 years for women aged 30-50 years, and every 3 years for those women living with HIV. CDC guidelines for HIV infected women also recommends initial pap smear test at HIV diagnosis followed by repeat pap smear tests after 6 months and then every year.
PAP SMEAR, HPV DNA TEST, VIA
Dr Joshi cautioned that pap smear is not a very sensitive test as its sensitivity varies between 40-60%. There is a 50% chance of missing abnormality, she said. She strongly recommended HPV DNA test as it is the most objective test and other tests are somewhat subjective.
Dr Joshi also stressed that using visual inspection with acetic acid (VIA), popularly known as table vinegar, to identify precancerous cervical lesions and provide treatment at the same visit using a freezing technique called cryotherapy, works wonders in resource limited settings like ours. A randomized controlled trial conducted in Tata Memorial Hospital showed that VIA resulted in 31% reduction in cervical cancer incidence. Dr Joshi added that VIA is not only simple and low cost test but consumables too do not cost more than INR 25-30 (less than USD 0.5). VIA can be performed by a trained healthcare worker or a nurse, has an improved sensitivity if followed by cytology, and results are available immediately. It offers an opportunity to begin treatment at the same clinic visit. However it may result in some overtreatment but overall is beneficial in terms of public health outcomes.
Dr Joshi also highlighted that VIA performs better in HIV infected women as compared to cytology probably due to large lesions that are fairly common in our setting. VIA based screening is a practical and feasible approach for HIV infected women. She agreed with Dr Palefsky that HPV vaccines are safe and immunogenic in HIV infected girls and young women.
Reference:
Bobby Ramakant, Citizen News Service – CNS
Source-Medindia