In Canada, Medical residents may work longer hours per shift and per week than their counterparts in Europe, Australia and New Zealand.
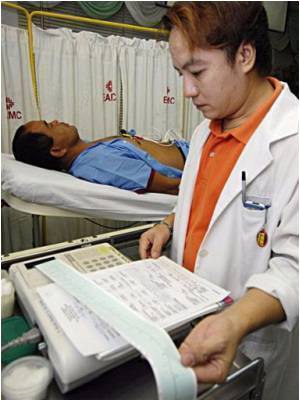
Her analysis of resident duty hours was published today in the Canadian Medical Association Journal (CMAJ).
Dr. Pattani said residents work an average of 60-90 hours a week in Canada under agreements negotiated between provincial residents' associations and employers. Residents are limited to 24 to 26 hours of consecutive work, except in Quebec, where on-call shifts were limited to 16 hours after a provincial arbitrator ruled in 2011 that a 24-hour shift posed a danger to residents' health and violated the Charter of Rights.
In New Zealand, residents are limited to 72 hours of work in a week and 16 hours of continuous work in any one shift. The Australian Medical Association has said that work in excess of 50 hours a week puts the resident at risk. The European Collective Agreement limits residents to 48 hours of work a week.
In the United States, senior residents may work up to 80 hours a week, averaged over four weeks and up to 24 hours continuously, but junior interns are limited to 16 hours of continuous work.
Last year a National Steering Committee on Resident Duty hours said the status quo in Canada was unacceptable and that shifts of 24 hours or longer without sleep should be avoided. It urged all provinces and health care institutions to develop comprehensive strategies to minimize fatigue and fatigue-related risks during residency.
"Although the National Steering Committee challenged the notion of a one-size fits all solution, in doing so it has left out important details, such as how individual residency programs should design fatigue risk management plans," Dr. Pattani and colleagues said. "Will scheduled naps during 24-hour call shifts be sufficient, or will residency programs inexorably move toward shifts that are no longer than 16 hours?"
A recent study by Dr. Najma Ahmed, a trauma surgeon at St. Michael's, also warned about strictly limiting the number of hours surgical residents can work, saying it has not improved patient outcomes but may have increased complications for some patients and led to higher failure rates on certification exams.
Dr. Pattani will attend Harvard University next year to study for her Master of Public Health, with a focus on Health and Social Behavior. She received a prestigious Frank Knox Memorial Fellowship for students from some Commonwealth countries.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email




