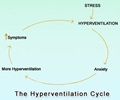
Researchers have long known that sleep-disordered breathing is associated with cardiovascular disease (CVD), but had no clue as to why.
They found that individuals with even modest levels of SDB (which describes a large proportion of the adult population) may have an enhanced pro-thrombotic biochemical profile, increasing their CVD risk.
Increased morning PAI-1 remained significantly associated with SDB severity in those with mild to moderate SDB even after taking into account evening PAI-1, suggesting that morning may be a reflection of overnight SDB-related physiologic stress, and indicating that PAI-1 may be a good biomarker for assessing SDB stress.
"In summary, these data suggest that, at low to modest levels of SDB, incremental increases in AHI are associated with increases in levels of two pro-thrombotic biomarkers associated with CVD. Future directions include exploring whether treatment of even mild to moderate levels of SDB improves biomarkers of thrombosis, and performing further work to understand the specific pathways and pathobiology of SDB-related increased risk of thrombosis," said Mehra.
John Heffner, M.D., past president of the American Thoracic Society, commented, "This study joins so many others that paint a consistent picture of sleep as a fundamentally important physiologic process for health that can negatively impact multiple organ systems when disordered breathing occurs."
The study appears online ahead of the print edition of the American Journal of Respiratory and Critical Care Medicine on the American Thoracic Society's Web site.
Advertisement