Report says patients in recovery from dependence on prescription pain medications may show signs that the body's natural reward systems are normalizing, within a few months after drug withdrawal.
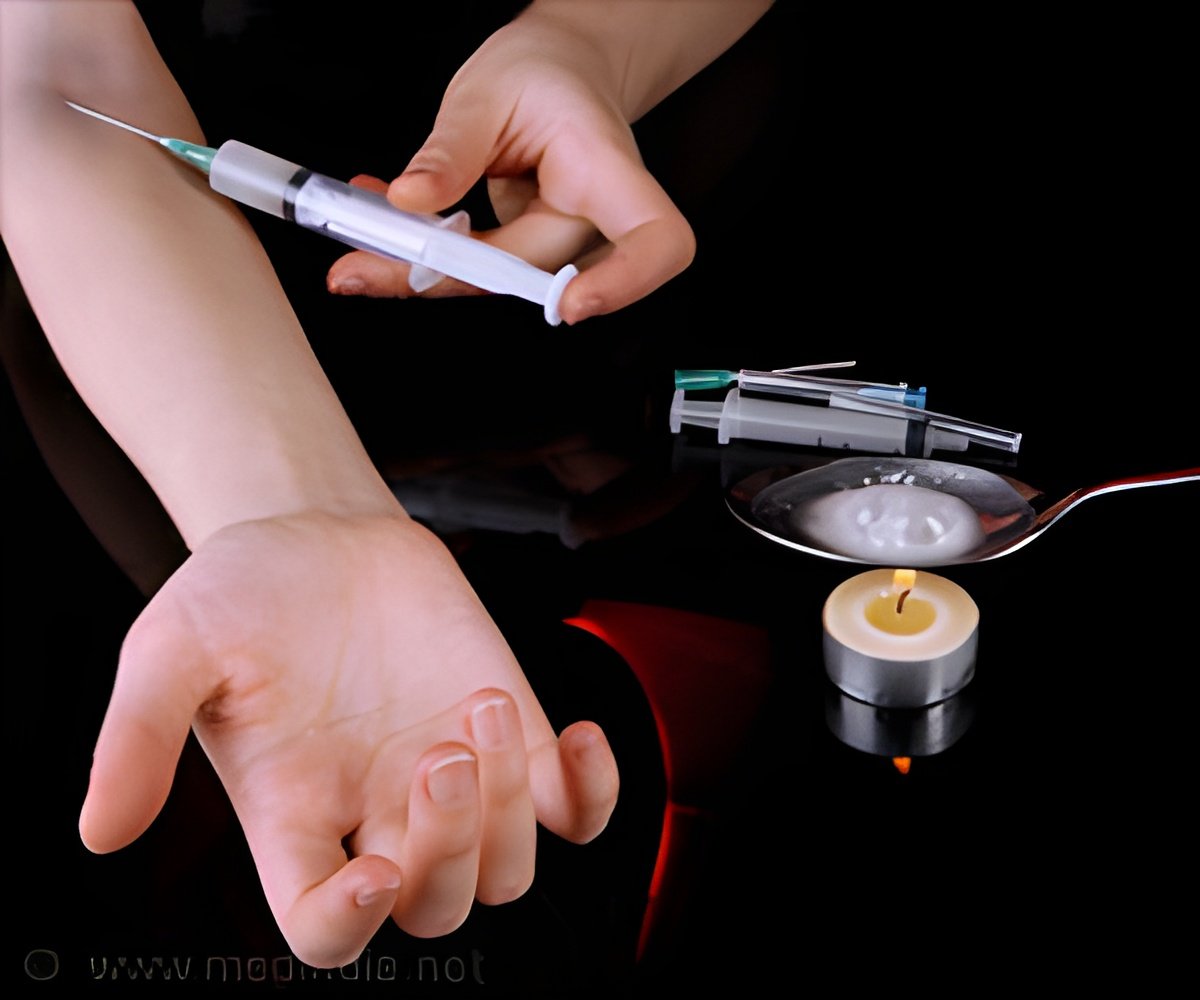
The pilot study included two groups of seven patients in residential treatment for dependence on opioid pain medications. One group had recently gone through medically assisted opioid withdrawal--within the past one to two weeks. The other group was in extended care, and had been drug-free for two to three months. A group of normal controls were studied for comparison.
The researchers performed several tests to assess changes in the "brain reward system" during early recovery. After drug withdrawal, many people with opioid dependence have "persistent changes in the reward and memory circuits" they may experience heightened "rewards" or "pleasure" in response to drugs and related stimuli, but greatly reduced responses to naturally pleasurable stimuli (such as good food, or friendship).
Dr Bunce explains, "This is thought to occur because opiates are potent stimulators of the brain's reward system; over time, the brain adapts to the high level of stimulation provided by opiates, and naturally rewarding stimuli can't measure up." Such dysregulation of the natural reward system may contribute to the high risk of relapse during recovery.
The test results showed several significant differences in the reward system between groups. A test of startle reflexes showed that patients with recent drug withdrawal had reduced pleasure responses to "natural reward" stimuli, for example, pictures of appetizing foods or people having fun.
In brain activity studies, patients with recent drug withdrawal showed heightened responses to drug-related cues, such as pictures of pills. In the extended-care patients, these increased responses to drug cues, in a region of the brain called the pre-frontal cortex, involved in attention and self-control, were significantly reduced.
All of these changes, brain and hormonal responses to drug cues and natural rewards, as well as sleep disturbances, were correlated with abstinence time. The more days since the patient used drugs, the lower the abnormal responses.
That's a potentially important step forward in addiction medicine research, Dr Bunce believes. "It shows that if the patient remains in treatment and off drugs for several months, the body's natural reward systems may have the capacity to return toward normal, making it easier for them to remain drug-free outside the treatment setting." With further study, tests of the natural reward system might provide useful, objective markers of recovery clinical tests that help to evaluate how the patient's recovery is proceeding.
Such tests might help in managing the difficult problem of prescription opioid dependence, an ongoing epidemic associated with a high risk of relapse after drug withdrawal. Dr Bunce and colleagues are conducting a follow-up study, funded by the National Institute on Drug Abuse, to determine whether measures of the brain's reward system, sleep and the stress response system indicate the capacity for re-regulation and the patient's risk of relapse during recovery.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email





