A quality improvement initiative improved the outcomes of patients undergoing cardiac surgery at select medical centers in northern New England.
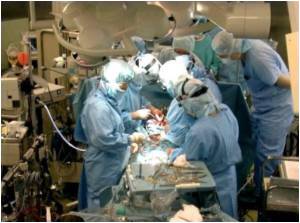
As part of the study, members of the Northern New England Cardiovascular Disease Study Group (NNECDSG) implemented a readiness bundle of preoperative interventions for urgent patients undergoing CABG surgery at eight medical centers in Maine, New Hampshire and Vermont.
The readiness bundle included seven evidence-based interventions:
- Preoperative use of aspirin (within seven days)
- Preoperative use of a beta-blocker (within 24 hours)
- Preoperative use of a statin-type lipid-lowering agent (within 24 hours)
- Preoperative hematocrit above 30 percent
- Glucose level less than 150 mg/dL at 6 a.m. on the day of surgery
- Delaying surgery a minimum of three days after an acute myocardial infarction
- Induction heart rate of less than 80 beats per minute
Lead author Kristine Chaisson, RN, BSN, CCRN, MS, executive director of the Heart and Vascular Center at Holy Cross Hospital in Fort Lauderdale, Florida, said, "It is both challenging and rewarding to implement evidence-based strategies into clinical practice with a team-based approach."
NNECDSG representatives examined data from the 150 most recent, urgent, isolated patients with CABG at each of the eight medical centers, for a total of 1,200 patients.
A scaled bundle score of 0 to 100 was calculated for each patient to represent the percentage of interventions applied.
Among the findings, patients with the highest scores had significantly shorter intubations and hospital stays. They were also at lower risk for morbidity and mortality.
The NNECDSG makes its data collection forms and definitions available online at www.nnecdsg.org. During the last 24 years, data on approximately 190,000 procedures have been collected and analyzed.
As the American Association of Critical-Care Nurses' bimonthly clinical practice journal for high acuity, progressive and critical care nurses, CCN is a trusted source for information related to the bedside care of critically and acutely ill patients.
Access the article abstract and full-text PDF by visiting the CCN website at www.ccnonline.org.
About Critical Care Nurse: Critical Care Nurse (CCN), a bimonthly clinical practice journal published by the American Association of Critical-Care Nurses, provides current, relevant and useful information about the bedside care of critically and acutely ill patients. The journal also offers columns on traditional and emerging issues across the spectrum of critical care, keeping critical care nurses informed on topics that affect their practice in high acuity, progressive and critical care settings. CCN enjoys a circulation of more than 100,000 and can be accessed at www.ccnonline.org.
About the American Association of Critical-Care Nurses: Founded in 1969 and based in Aliso Viejo, Calif., the American Association of Critical-Care Nurses (AACN) is the largest specialty nursing organization in the world. AACN joins together the interests of more than 500,000 acute and critical care nurses and claims more than 235 chapters worldwide. The organization's vision is to create a healthcare system driven by the needs of patients and their families in which acute and critical care nurses make their optimal contribution.
Source-Newswise
 MEDINDIA
MEDINDIA


 Email
Email








