‘Immunotherapy may be useful for colorectal cancer prevention in certain high-risk groups.’
Tweet it Now
"Our question was how this worked in premalignancy," said senior author Eduardo Vilar-Sanchez, M.D., Ph.D., assistant professor of Clinical Cancer Prevention and Gastrointestinal (GI) Medical Oncology. "Can we apply checkpoint inhibitors or checkpoint inhibitor strategies to prevent MMR-deficient colorectal cancer?"
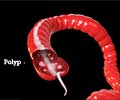
Lynch syndrome (LS), which is caused by inherited mutations in MMR, provides the perfect context in which to study early immune activation and explore the potential use of checkpoint inhibitors in a prevention setting, explained Vilar-Sanchez. Over 1 million people in the U.S. are affected by LS, the most common hereditary colorectal cancer syndrome. In the study, the researchers analyzed gene expression to characterize the immune profile in 11 polyps and three early-stage tumors from 14 patients with LS. As a control, the researchers also analyzed 17 polyps from patients with Familial Adenomatous Polyposis (FAP), a hereditary colorectal cancer syndrome which does not exhibit MMR deficiencies. The resulting profiles revealed increased expression of several markers of immune activation, including CD4 T-cells, proinflammatory molecules and checkpoint molecules, such as PD-L1 and LAG-3, in LS polyps compared to FAP polyps. However, contrary to traditional models of immune activation, the observed immune profiles were independent of the rate of mutations or neoantigens present in the sample.
"To our surprise, our findings don't follow the standard model. The majority of premalignant lesions do not have an excessive increase in mutations or neoantigens," said Vilar-Sanchez. "However, we observed there is already immune activation, meaning the activation precedes the development of the mutations." The findings suggest a baseline level of immune activation exists in precancerous polyps, which may prime them for susceptibility to checkpoint blockade, explained Vilar-Sanchez.
Future work will be necessary to clarify the mechanism by which this immune activation occurs, as the current study was observational in nature. The researchers hope to initiate clinical studies to investigate the use of checkpoint blockade strategies for preventing colorectal cancer in high-risk groups, such as those with LS. "Lynch syndrome patients have a strong immune activation in the colon, and that immune activation can be exploited for preventive purposes," said Vilar-Sanchez. "I think our data provide the information needed to launch studies to use checkpoint inhibition in the setting of prevention."
Source-Eurekalert