Peripheral nerve blockers are medications often added in order to reduce pain and the need for active pain killers such as opioids.
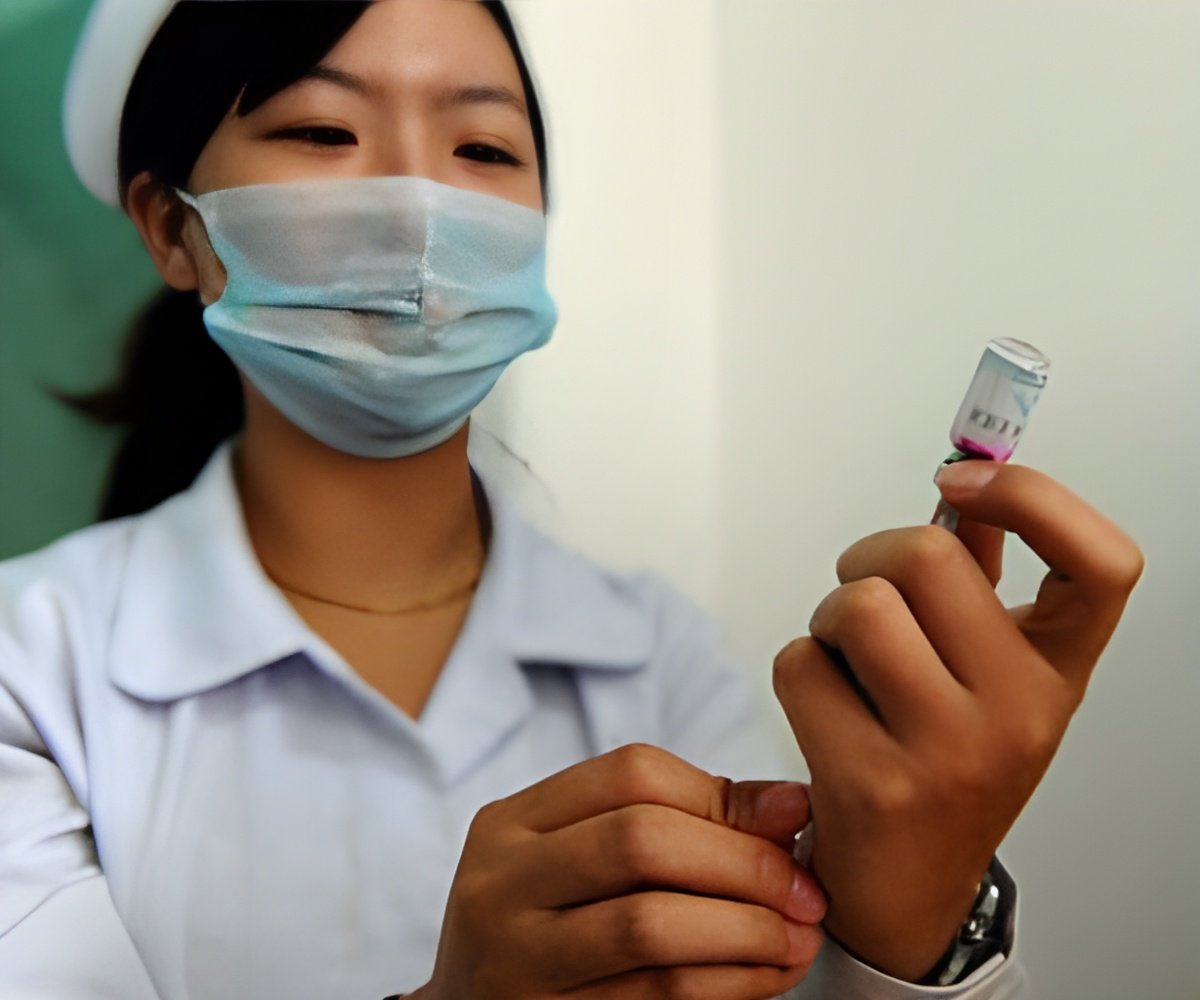
TOP INSIGHT
Peripheral Nerve Blockers involve injecting medication around specific nerves to targeted areas during hip or knee replacement surgeries.
A team of researchers looked at more than 1 million cases of hip and knee arthroplasty over a 7-year period. They compared the rate of complications such as heart attack; lung, gastrointestinal, and kidney complications; stroke; infection; wounds; clots; inpatient falls; and mortality in those receiving a PNB to those without the intervention. They also looked at resource utilization such as the need for blood transfusion, admission to intensive care, opioid consumption, length of stay, and cost of hospitalization.
In terms of both complications and resource utilization, PNBs were associated with better outcomes than when the intervention was not used irrespective of anesthesia type chosen. The researchers concluded that increased use of PNBs in patients receiving knee and hip reconstruction and replacement could have a significantly positive impact on medical and economic outcomes.
Source-Newswise
 MEDINDIA
MEDINDIA

 Email
Email