Medical practioners say that many women suffer from painful periods and other issues , unnecessarily. Most have problems like copious bleeding, debilitating pain, out-of-control PMS, or annoyances like constipation or diarrhea. Yet, very few women know that medical science and technology has advanced so much as to actually provide quick fixes to this age-old bane of womanhood.
Heavy bleeding, also called menorrhagia, is common among many women. (The average woman loses about three to four tablespoons per cycle; more than five tablespoons is considered heavy).One such is the procedure to help here is NovaSure. Here the uterine lining is removed by a wand inserted into the uterus through the cervix. It emits energy that, in most cases, permanently removes the uterine lining. This results in the cessation of periods, altogether.
The five-minute procedure is done in a gynecologist’s office. Many women report lighter bleeding right away. And a recent study found that after seven years, more than 95 percent stopped having periods. For those past the child-rearing age or those who want to do away with periods altogether, where heavy bleeding actually makes their life unbearable, NovaSure is a prayer answered.
The 365-day Pill, called Lybrel, approved by the FDA, is another way to skip monthly menstruation. Yet, since Lybrel contains estrogen, it’s not for recommended for women who are prone to blood clots, such as smokers; who get migraines with an aura; or who are over age 35 with elevated heart disease risks).
For just lessening the intensity of period bleeding, the traditional Pill is enough. Its constant level of progesterone causes the endometrium to develop a much thinner lining.
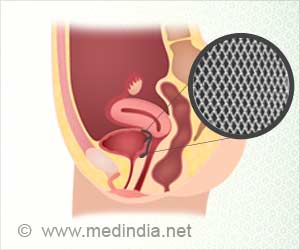
Another option is Mirena. Here the intrauterine device secretes progestin on a daily basis, thinning the uterine lining so there’s virtually nothing to shed.
Advertisement
Period pain can be helped with naproxen, aspirin, and ibuprofen. Here, they short-circuit the production of pain-causing chemicals called prostaglandins that are involved in muscle contractions. They work best if you start an hour before your cramps hit. “Load up with a double dose and keep the blood level up,” Haas suggests. (The maximum safe daily dose of ibuprofen is 2,400 milligrams, or 12 200-mg pills. Some doctors suggest starting with 800 mg and then taking 600 mg every six hours. Still, they suggest a talk with the doctor if a patient has elevated heart disease risks. The Food and Drug Administration (FDA) has recently reported that all NSAIDs, except aspirin, may heighten cardiovascular risks. The extended use of high dosages of aspirin or NSAIDs may cause gastrointestinal troubles, as well.
Advertisement
About two-thirds of regularly menstruating women have premenstrual symptoms(PMS), says Jean Endicott, PhD, director of the Premenstrual Evaluation Unit at Columbia University’s College of Physicians and Surgeons. Symptoms range from headaches, breast tenderness to unpleasant mood swings. Up to 8 percent of women who have PMS suffer mood changes severe enough to cause problems in their personal lives and daily routines; this more serious version of PMS is called premenstrual dysphoric disorder (PMDD).
For this, calcium supplements are a good first thing to try, Endicott suggests, because research shows they ease symptoms. Calcium may help even out hormone levels, say some experts. Endicott suggests 1,200 mg daily. “It should help take the edge off” over time, she says.
Daily exercise—like fast walking, lifting weights, or even dancing—may be the last thing you want to do when in the throes of PMS, but it has proven antidepressant and anti-anxiety effects.
Antidepressants (like Paxil, Prozac, Sarafem, and Zoloft) can relieve severe symptoms. Another choice is Yaz, a birth-control pill, which is FDA-approved to treat PMDD. Clinical trials show it can cut symptoms by at least half, though the reasons are unclear.
Many women have diarrhea, gas, or constipation during their periods. Prostaglandins, the chemicals that cause cramping in your uterus, do the same in your bowels. “For lots of women, it’s common to have a loose stool or diarrhea on the day they have a lot of bleeding,” says Leslie Miller, University of Washington–Seattle clinical associate professor of obstetrics and gynecology.
Gynecologists suggest fiber to help keep GI issues under control. They advice to aim for 30 grams a day from cereal, fruit with the skin, and vegetables. They caution against adding fiber to the diet too fast during periods; as this could worsen diarrhea. For constipation, Miller advises women not to hold in bowel movements. Ibuprofen and other similar anti-inflammatory medicines may reduce gastro cramping. To avoid tummy irritation, take it with food.
For some women who experience a combo of excessive bleeding, cramping, breast tenderness, headaches, PMS, and other troubles, Miller advises continuous birth control pills—you just skip the placebo week and move on to your next pack, she informs. She also suggests considering NovaSure.
Source-Medindia
ANN/J