People with ankle injuries who do not respond successfully to initial treatment may have a second chance at recovery, thanks to two new procedures developed to restore the injured area.
People with ankle injuries who do not respond successfully to initial treatment may have a second chance at recovery, thanks to two new procedures developed to restore the injured area.
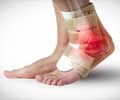
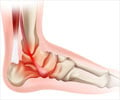
The study is published in the July 2009 issue of the Journal of the American Academy of Orthopedic Surgeons (JAAOS).The study reviews emerging techniques that have proven successful in treating injuries to the talus, the small bone, which is located between the heel bone and the lower bones of the leg. The talus helps form the ankle joint.
Although most injuries to the talus can be successfully treated using traditional "first-line" therapies involving removal of dead tissue (called "debridement") and drilling, about one-fifth to one-quarter of people with ankle injuries need additional "second-line" restorative treatment to heal successfully, said lead author Matthew Mitchell, MD, an orthopedic surgeon in private practice in Casper, Wyoming.
The two new techniques rely on cells grown in a lab, and eliminate the need for ostetomy (cutting the bone of the tibia) in some cases, he said. Autologous chondorcyte implantation, or ACI, involves removing cartilage cells from the knee or the ankle and growing them in a lab. Once grown, the cartilage is transplanted to the talus. ACI usually involves an ostetomy in order to implant the cells. In matrix-induced autologous chondrocyte implantation, or MACI, cells are grown on a special backing material, or "matrix," and then transplanted to the talus. In the authors' experience, an osteotomy is not necessary to implant the cells.
Of these two techniques, the newer MACI technique may offer the most benefits to the patient, according to Dr. Mitchell.
"Both ACI and MACI show a lot of promise, but I think the advantage of MACI is that an osteotomy is not necessary in order to successfully implant the matrix," he said. "You only need to make an incision to place the graft, which decreases the morbidity of the procedure quite a bit."
Traditional restorative techniques involve removing a cartilage donor plug from the knee and implanting it over the ankle injury, or "lesion." This requires an operation on the knee and cutting the bone (osteotomy) of the tibia to accommodate the graft.
"In most individuals, results are favorable with reparative techniques, such as debridement and drilling," said Dr. Mitchell. "The lesions that are problematic and which don't respond well to reparative treatments are lesions that are larger, and those which are fairly deep, as well as lesions which have a cyst-like structure. Whether or not an ankle "lesion" requires additional treatment after an initial reparative procedure often depends upon several factors, including: size, depth and structure of the legion.
"Once you've performed a reparative technique and the patient still doesn't heal properly, then we would move on to a second-line restorative treatment," he said.
Source-Eurekalert
ARU
 MEDINDIA
MEDINDIA



 Email
Email