New imaging agent can safely show engraftment after hematopoietic stem cell transplant as early as days after the transplant.
TOP INSIGHT
New imaging test called 18F-fluorothymidine allows the newly infused developing immune system and marrow to be readily visible after a hematopoietic stem cell transplant.
As they wait in the protected confines of a hospital, patients who undergo HSC transplants receive blood tests every day to gauge successful engraftment, searching for the presence of immune cells called neutrophils, explains Kirsten M. Williams, M.D., blood and bone marrow transplant specialist at Children's National Health System.
"As you head into week three post-transplant and a patient's cell counts remain at zero, everyone starts to get nervous," Dr. Williams says. The longer a patient goes without an immune system, the higher the chance that they'll develop a life-threatening infection. Until recently, Dr. Williams says, there has been no way beyond those daily blood tests to assess whether the newly infused cells have survived and started to grow early healthy cells in the bone marrow, a process called engraftment.
The study evaluated an investigational imaging test called 18F-fluorothymidine (18F-FLT). It's a radio-labeled analogue of thymidine, a natural component of DNA. Studies have shown that this compound is incorporated into just three white blood cell types, including HSCs. Because it's radioactive, it can be seen on various types of common clinical imaging exams, such as positron emission tomography (PET) and computed tomography (CT) scans. Thus, after infusion, the newly infused developing immune system and marrow is readily visible.
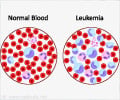
To see whether this compound can readily and safely visualize transplanted HSCs, Dr. Williams and colleagues tested it on 23 patients with various forms of high-risk leukemia.
Each of these patients had successful engraftment, reflected in blood tests two to four weeks after their HSC transplants. However, the results of the imaging exams revealed a far more complicated and robust story.
Interestingly, notes Dr. Williams, this pathway is the same one that HSCs take in the fetus when they first form. Although experimental model research had previously suggested that transplanted HSCs travel the same route, little was known about whether HSCs in human patients followed suit.
The study also demonstrated that the radiation in 18F-FLT did not adversely affect engraftment. Additionally, images could identify success of their engraftments potentially weeks faster than they would have through traditional blood tests--a definite advantage to this technique.
"Through the images we took, these patients could see the new cells growing in their bodies," Dr. Williams says. "They loved that."
Besides providing an early heads up about engraftment status, she adds, this technique also could help patients avoid painful bone marrow biopsies to make sure donor cells have taken residence in the bones or at the very least help target those biopsies. It also could be helpful for taking stock of HSCs in other conditions, such as aplastic anemia, in which the body's own HSCs fade away. And importantly, if the new healthy cells don't grow, this test could signal this failure to doctors, enabling rapid mobilization of new cells to avert life-threatening infections and help us save lives after transplants at high risk of graft failure.
"What happens with HSCs always has been a mystery," Dr. Williams says. "Now we can start to open that black box."
Source-Eurekalert
 MEDINDIA
MEDINDIA
 Email
Email










