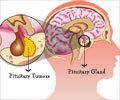
Surgery is the primary treatment for pituitary adenomas, followed by radiation therapy, but too much radiation can affect the optic system and damage vision.
TOP INSIGHT
Radiation oncologists strategized on using fractionated stereotactic radiotherapy as the best way to kill pituitary gland tumors.
FSRT is a treatment given in multiple small doses over a period of time. Considered a variation of the traditional stereotactic radiosurgery (SRS), FSRT can treat the pituitary adenomas more aggressively than a single dose and with less complications than SRS.The Houston Methodist study not only supported this, Baskin said, but demonstrated that FSRT actually beat both SRT and conventional radiotherapy at long-term effectiveness. Surgery is the primary treatment for pituitary adenomas, followed by radiation therapy, but too much radiation can affect the optic system and damage vision.
"We treated and followed 75 patients who underwent FSRT for a residual pituitary adenoma between 2004 and 2013," said Bin Teh, M.D., vice chair of Houston Methodist's Department of Radiation Oncology and co-author on the Neurosurgery paper. "None of them experienced any tumor recurrence during our monitoring period and nearly 70 percent of those with hormonal imbalances caused by the adenomas returned to normal levels."
Further studies will investigate the long-term (10 years or greater) safety and efficacy of FSRT in larger groups of patients. "We also plan to conduct prospective research that will evaluate FSRT and SRT so that the benefits and limitations of both therapies in treating pituitary adenomas can be directly compared," said Baskin, director of the Kenneth R. Peak Brain and Pituitary Tumor Center at Houston Methodist Hospital.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email