Women with chronic heart failure survive longer as compared to their male counterparts, researchers have said.
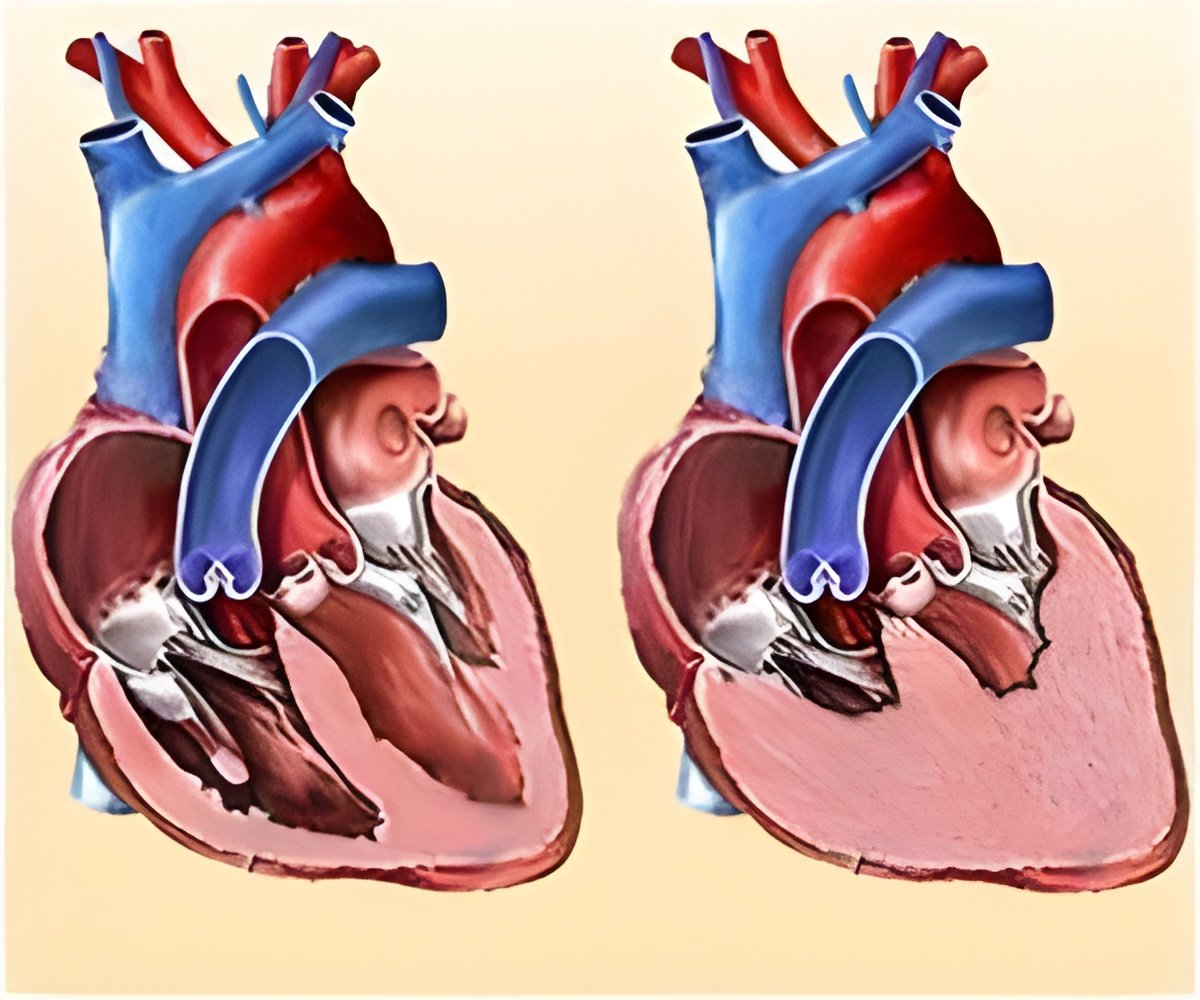
Heart failure is by far the single biggest reason for acute hospital admission. Its incidence is still increasing - more cases are being identified, more people are living to an old age, and more are surviving a heart attack but with damage to the heart muscle.
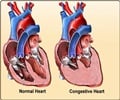
The condition arises when the heart fails to pump sufficient blood to meet the body's demands. The common symptoms of heart failure - shortness of breath, tiredness, oedema - are usually associated with failure of the left side of the heart, as defined by a measurement known as left ventricular ejection fraction.
The latest study also found that heart failure patients whose ejection fraction is not reduced have a lower mortality risk that those with reduced ejection fraction.
According to the authors, preserved ejection fraction is more common among women than men, and this "may be expected to lead to better survival for these patients".
The study analysed data from 31 randomised and observational studies involving 28,052 men and 13,897 women with chronic heart failure.
When adjusted for age, however, the results showed that men had a 31 percent higher risk of death than women, and that male gender was an independent risk factor for death at three years.
This excess mortality risk associated with male gender was of similar magnitude in patients with either reduced or preserved ejection fraction, which was not affected by either age or history of hypertension.
"This study has clearly demonstrated that survival is better for women with heart failure than for men, irrespective of ejection fraction, age or other variables," Manuel Martinez-Selles, first author of the study from the Gregorio Maranon University Hospital in Madrid, said.
"This survival benefit is inherent to female sex and there are a number of potential explanations for the better outcomes in women. The female heart appears to respond to injury differently from the male heart.
For example, women have less ventricular remodelling, greater preservation of right ventricular function, and greater protection against ventricular arrhythmias, neurohormonal activation, genetic mutations, and apoptosis. Some of these advantages could be related to pregnancy and to sex-specific differences in gene expression," Martinez-Selles added.
The study has been published in the European Journal of Heart Failure.
Source-ANI
 MEDINDIA
MEDINDIA

 Email
Email