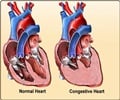
Medicare expenses for patients suffering from acute myocardial infarction (AMI, heart attack) saw a substantial increase between 1998 and 2008.
Donald S. Likosky, Ph.D., of the University of Michigan, Ann Arbor, and colleagues compared expenditures by analyzing a sample of Medicare beneficiaries hospitalized with AMI in 1998 and 1999 (n=105,074) and in 2008 (n=212,329).
Researchers found a decline in the number of hospitalizations for AMI, but overall expenses per patient increased by 16.5 percent (absolute difference, $6,094). Of the total increase in expenses, 25.6 percent was for care within 30 days of the date of hospitalization and 74.4 percent was for care one month to one year after. Medicare spending per patient increased by $1,560 within the first 30 days after hospitalization and by $4,535 within 31 to 365 days. Expenses for skilled nursing facilities, hospice, home health agencies, durable medical equipment and outpatient care nearly doubled 31 days or more after hospital admission, according to study results. Results also show mortality within one year of an AMI declined from 36 percent in 1998 through 1999 to 31.7 percent in 2008.
The authors suggest that although Medicare's current bundled payments may limit spending for patients with AMI within 30 days of the episode, they do not contain spending beyond 30 days, which accounted for most of the expenditure growth.
"This growth in the use of health care services 31 to 365 days after an AMI challenges efforts to control costs. A potential approach is to extend bundled or episode-based reimbursements to periods beyond 30 days," the study concludes.
(JAMA Intern Med. Published online September 23, 2013. doi:10.1001/jamainternmed.2013.10789. Available pre-embargo to the media at http://media.jamanetwork.com.)
Advertisement
Commentary: Going After the Money, Curbing Medicare Expenditure Growth
Advertisement
"The study by Likosky et al, as well as other recent evidence, should be a wake-up call for federal policy makers. Most of Medicare's current efforts to curtail unnecessary spending, including readmissions and bundled payments, are focused on the first 30 days after admission; only a few programs extend the focus to 90 days," Jha continues.
"The study by Likosky et al is a timely reminder of the importance of research and data for policy making. Refocusing on services following early post-acute services should be straightforward," Jha concludes.
(JAMA Intern Med. Published online September 23, 2013. doi:10.1001/jamainternmed.2013.7081. Available pre-embargo to the media at http://media.jamanetwork.com.)
Editor's Note: Please see the article for additional information, including other authors, author contributions and affiliations, financial disclosures, funding and support, etc.
Source-Eurekalert