Tumor suppressor gene folliculin is essential to normal lung function in patients with Birt-Hogg-Dube syndrome, reveal researchers at Penn Medicine.
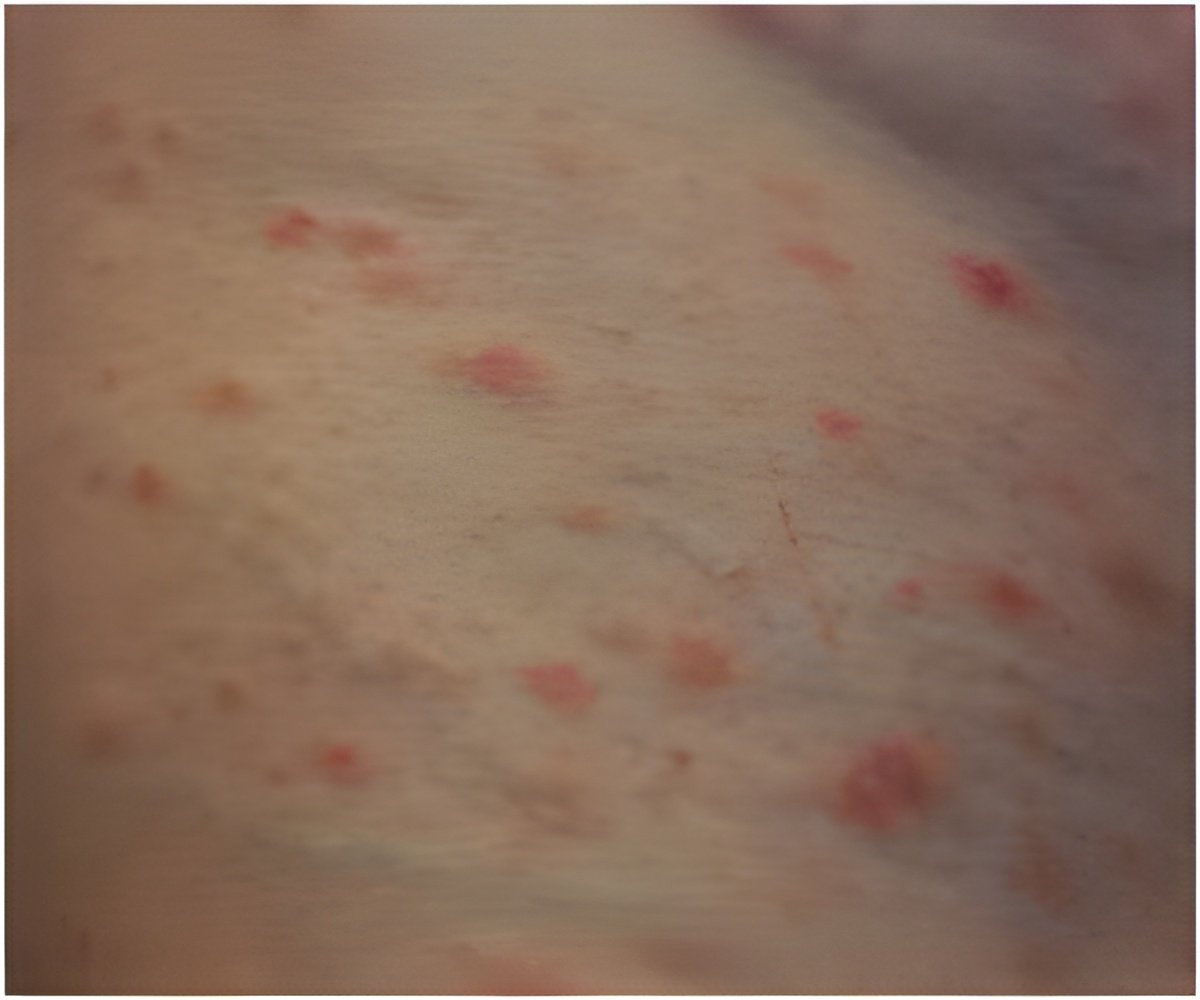
Between 80 and 100 percent of patients with BHD will develop multiple holes or cysts in the lung.
Healthy human alveoli, the terminal ends of the respiratory tree, are lined with type I and type II alveolar epithelial cells (AECs), a renewable population of progenitors in these distal airspaces. AECs are known to maintain pulmonary alveolar homeostasis by regulating gas exchange and fluid transport in the lungs.
Previous studies have shown that there might be some crosstalk between FLCN and the master energy sensor AMP-activated protein kinase (AMPK). AMPK maintains epithelial cell to cell interactions and is essential for epithelial cell survival. It is regulated through LKB1, a tumor suppressor gene associated with 30 percent of lung cancers. E-cadherin, the "zipper" molecule that connects epithelial cells, directs LKB1 to cell junctions and its loss impairs LKB1-mediated AMPK activation. This implies that a loss of or mutation in FLCN can trigger a reaction that can impair AMPK activation, epithelial cell to cell interaction and structure, and as a result, promotes cell death.
Penn researchers set out to examine this hypothesis to determine how and why this occurs.
Krymskaya and her team tested both deleted FLCN in mouse lung type II alveolar epithelial cells and mutated FLCN that lacked normal function in both humans with BHD and mouse epithelial cell systems, and compared them with normal human and mouse control cells.
Next, to evaluate the role of FLCN in the lung, the team isolated the alveolar epithelial cells from the mice with FLCN and deleted the gene in vitro to show the decreased cell to cell interactions and increased cellular permeability. They also examined activity of AMPK in these cells and saw that cells were dying without FLCN, so there was not proper activation of AMPK.
Further, the Penn researchers are the first to demonstrate the mechanism by which FLCN begins the domino effect necessary for normal lung function. Examination of cells with FLCN mutations shows that FLCN downregulates E-cadherin and LKB1 which controls AMPK activity. FLCN also maintains alveolar surface tension preventing the lungs from collapse, as seen in BHD disease. Without this, the lung changes associated with BHD and other common and rare lung diseases begin to appear: the abnormal enlargement of airspaces among them.
The team then showed that in fact, AMPK is necessary for epithelial cells survival. Importantly, using mouse BHD model, investigators show beneficial effect of pharmacological activator of AMPK AICAR, an AMPK stimulator, on lung function.
"AMPK is the metabolic regulator of the alveolar epithelial cells," says Krymskaya. "We may be able to reverse cell death if we can find a way to activate AMPK therapeutically in patients with less than optimal or mutated FLCN."
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email






