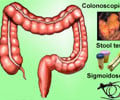
Participation in colorectal cancer screening is low and the use of colonoscopy is infrequent among African Americans despite similar access to care across races in Veterans Affairs healthcare system.
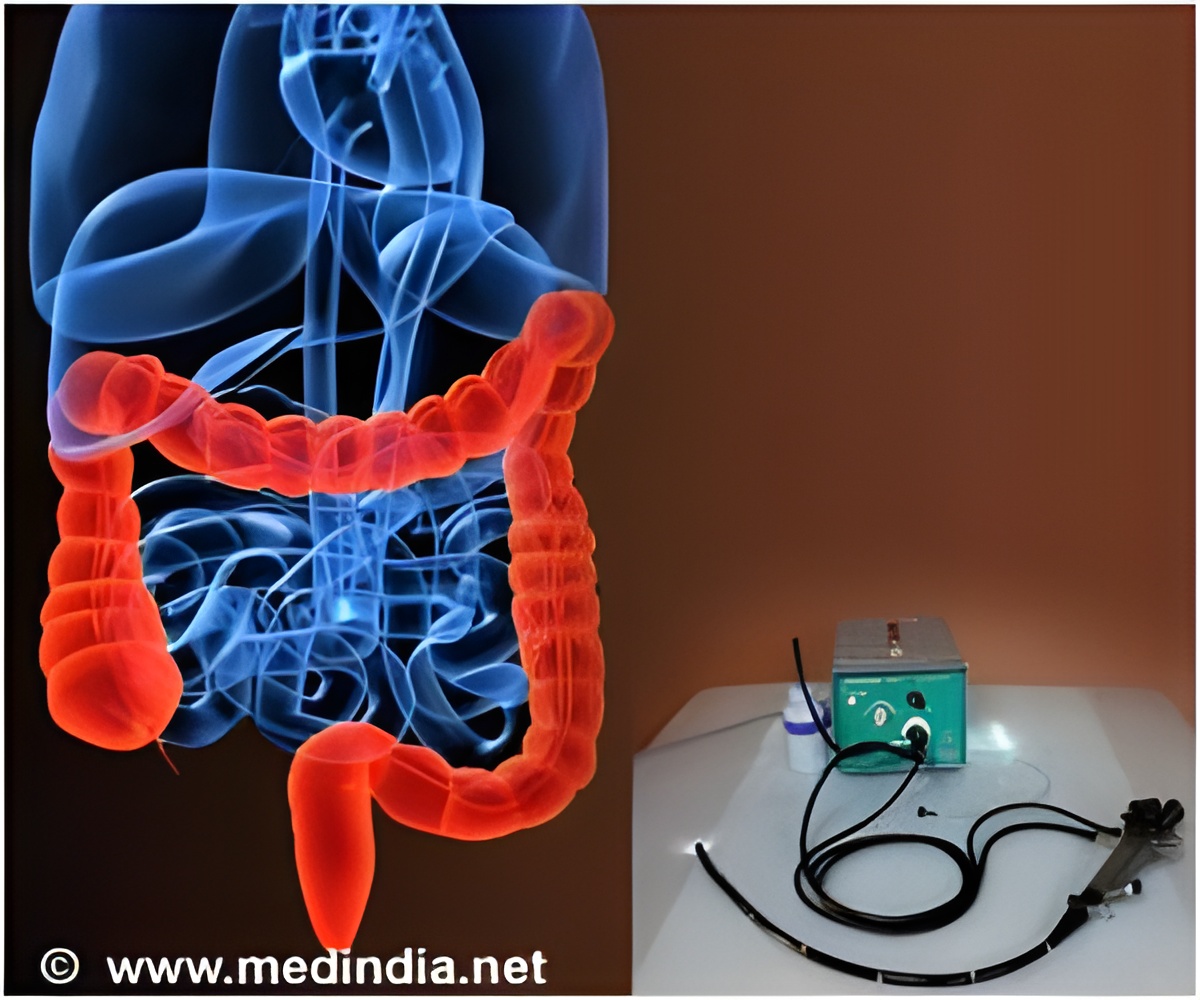
The specific causes of CRC outcome inequalities in African Americans are not fully characterized. Biological susceptibility, a diet higher in fats and red meats, increased likelihood of smoking, social and economic disparities, and low use of screening methods have been implicated as potential contributing causes. Particular attention has been paid to low adherence to screening guidelines among African Americans, and multiple studies demonstrate that African Americans are less likely to engage in CRC screening than non–African Americans.
The Veterans Affairs (VA) health system presents an ideal model to test whether patient and provider factors affect CRC screening after controlling for system-level factors. Because access inequalities are minimized in the VA setting and given recent studies indicating fewer disparities in CRC treatment in VA settings, it is possible that CRC screening rates are equal among races in the VA population. However, the extent to which disparities in screening adherence currently exist in the VA population is unknown.
"We aimed to determine the rates of screening uptake and time to screening uptake in African American and non–African American veterans in a large VA health care system database. In addition, we sought to identify modifiable predictors of CRC screening in non–African American and African American veterans by using a conceptual framework accounting for a wide range of clinical and demographic characteristics," said study lead author Fola May, MD, MPhil, VA Greater Los Angeles Healthcare System. "We found marked disparities in CRC screening despite similar access to care across races. Participation in screening remained low and use of colonoscopy was infrequent despite current guidelines aimed at increasing CRC screening in African Americans. When adjusting for race, homelessness, low service connectedness, and greater use of prescription drugs, the lack of a primary care visit within two years of CRC screening eligibility independently predicted low screening. Notably, individuals with a primary care visit within two years of CRC screening eligibility were nearly four times more likely to have had at least one CRC screening test."
Methods The researchers sought patients receiving care in the VA Greater Los Angeles Healthcare System, an integrated network of 12 sites serving a racially- and ethnically-diverse population in Southern California. A random number generator was used to identify African American patients older than 45 years of age and non–African Americans older than 50 years of age and data was extracted from the VA's electronic medical records. Included subjects were eligible for initial CRC screening between January 1996 and October 2012. Before January 2009, all subjects were considered screening-eligible after their 50th birthday. Because of new screening recommendations for African Americans in the 2009 American College of Gastroenterology (ACG) CRC screening guidelines, researchers also included African Americans who turned 45 years of age after 2009.
The main outcome measurements were the uptake of any screening method; uptake of colonoscopy, in particular; predictors of screening; and time to screening in African Americans and non–African Americans.
The researchers concluded that their analysis suggests that disparities in CRC screening between African Americans and non–African Americans exist in a large, urban VA health care network. These inequities in health exist in a patient population that has the same source and, presumably, access to health care. These findings confirm the need for focused and targeted efforts to address barriers to screening and especially screening colonoscopy in African Americans. The findings also highlight that having established primary care at the time of screening eligibility plays a significant role in screening uptake. The researchers noted that as insurance coverage is extended to all Americans, it will be important to emphasize regular use of health care services in middle-aged adults and knowledge about the benefits of screening to increase CRC screening in African Americans and overall.
 MEDINDIA
MEDINDIA

 Email
Email