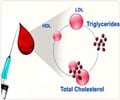
‘Lipids like cholesterol are a risk factor for many metabolic diseases including cardiovascular disease, hepatitis, and rare genetic disorders.’
Tweet it Now
Rare inherited mutations in the DYSF gene cause deficiencies in the protein dysferlin, resulting in debilitating limb-girdle muscular dystrophy type 2b. To date, there are no approved therapies for dysferlinopathies. Drug development has been slowed, in part, by the lack of animal models that closely mimic human symptoms. A new paper in the Journal of Lipid Research, however, reports the creation of a mouse that comes closer than its predecessors and contemporaries. A research team led by Pascal N. Bernatchez at the University of British Columbia in Canada set out to create the new mouse model after observing that elevated so-called "bad" cholesterol levels correlate with disease severity in some muscular dystrophy patients. While mice with the DYSF gene knocked out display muscle degradation, they usually don't lose the ability to walk like human patients do. Bernatchez's team knocked out both the DYSF gene and the apolipoprotein E gene in their mice. Loss of apolipoprotein E function increases bad cholesterol. The team's double-knockout mice developed more dramatic muscle wasting than mice with only DYSF knocked out and eventually were unable to walk. The researchers are hopeful that their new model will help scientists better understand the human disease. Importantly, the researchers wrote, though it's unclear at this stage precisely how bad cholesterol exacerbates muscle damage, their model revealed "a striking correlation" that deserves further investigation. The work was supported by the Jain Foundation. Alcohol consumption plus hepatitis B raises cholesterol in mice
Though a safe and effective vaccine for hepatitis B is available and used worldwide, the World Health Organization estimates that still some 257 million people are living with the viral infection. The virus is treatable but still causes liver scarring and in some cases liver cancer. Intravenous drug users who share needles are especially at risk of infection and are likely to abuse multiple substances, including alcohol, which causes liver damage as well. Given that damage to the liver affects how the organ creates and clears cholesterol and given that studies have found that hepatitis B alone and alcohol alone affect cholesterol homeostasis, a research team led by Qin Ning at Tongji Hospotal at Huazhong University of Science and Technology in Wuhan China wanted to learn more about the combined effects of hepatitis B and alcohol consumption on cholesterol deposition in the liver. In a new paper in the Journal of Lipid Research, the team reports that the virus and alcohol have a "synergistic effect" on cholesterol metabolism. That is to say that the combination increases cholesterol biosynthesis, decreases cholesterol utilization and impairs cholesterol uptake. To figure this out, the team created a mouse model with chronic hepatitis B and administered it ethanol. This resulted in increased cholesterol accumulation in the liver. Later experiments, using only cells, produced results that the researchers say indicate it is the HBc protein specifically that activates cholesterol biosynthesis and inhibits cholesterol degradation in the presence of alcohol.
Bacterial lipids lurk in healthy arteries
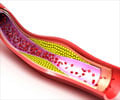
Perhaps you have heard that brushing your teeth can be good for your heart. Bacteria of the Bacteroidetes phylum may be the main culprits behind the association between gum disease and atherosclerosis, the accumulation of plaque in the arteries that can lead to heart attack or stroke. In a recent paper in the Journal of Lipid Research, researchers from the University of Connecticut reported on their investigation into how Bacteriodetes in the mouth and gut may contribute to the development of atherosclerosis. They found deposits of a lipid made by these bacteria in the wall of healthy carotid arteries. A human enzyme can convert the bacterial lipid into a closely related molecule that is known to trigger inflammation. Patients with atherosclerosis, who were undergoing surgery to reduce the risk of stroke, had much more of the modified, inflammation-associated molecule than the original lipid. The study's senior author, Frank Nichols, told ASBMB that "Many think that atherosclerosis is caused by eating fatty foods, but it is now apparent that other lipids produced by oral and intestinal bacteria accumulate in diseased arteries." It remains to be determined whether accumulation of the original lipid and conversion to the inflammatory molecule can cause heart disease, or are a side effect.
Advertisement
Source-Eurekalert