The first person to be treated with CTL019 has recently marked five years cancer-free. Two others have made it to four and half years with no sign of return of the cancer. The fourth patient had been in remission for 21 months, and then died of an infection following a surgery that was unrelated to the leukemia. Four of the patients (29%) responded to the therapy, for a median of seven months, but their cancer eventually returned.
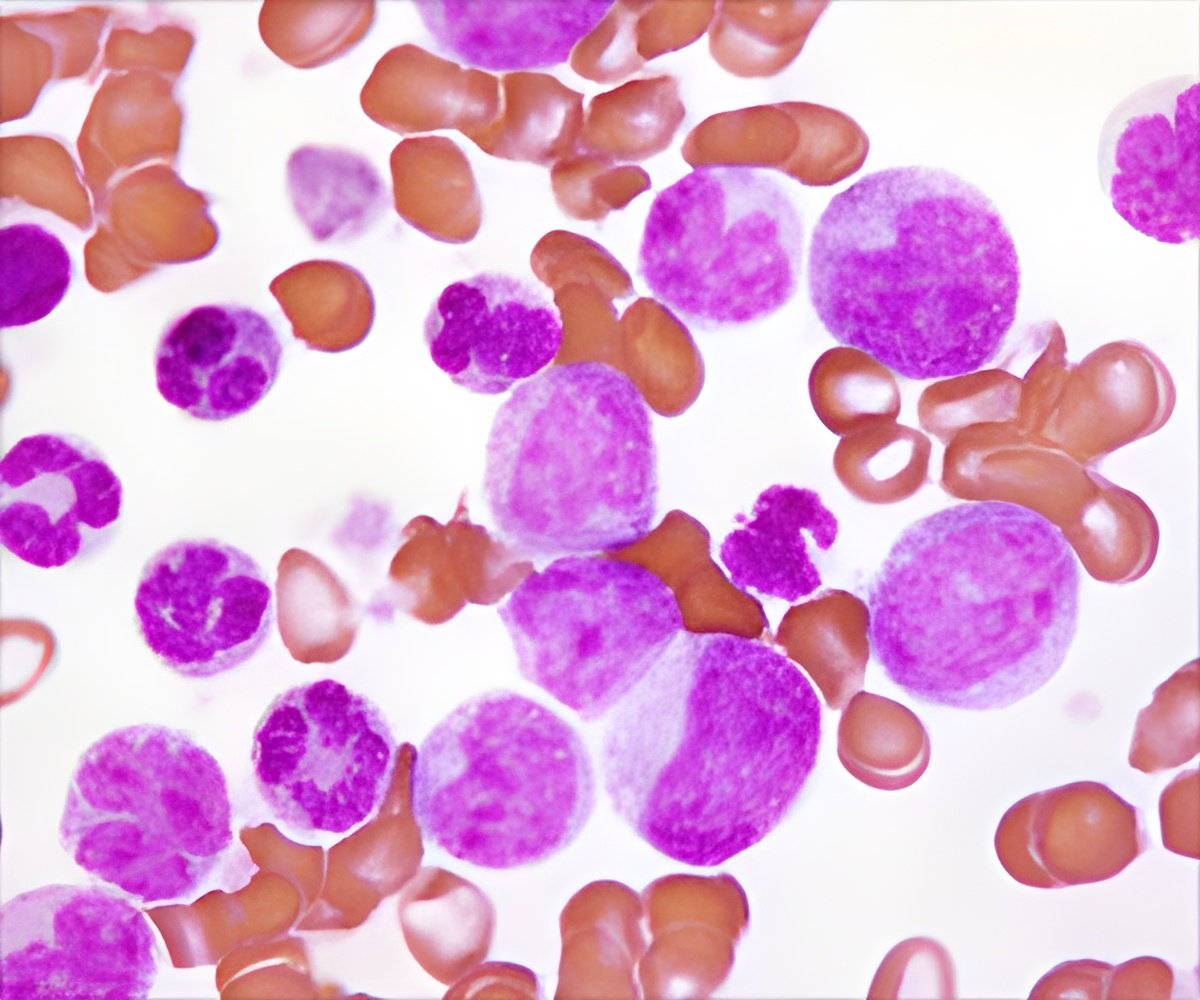
The experimental therapy involves collection of T-cells from cancer patients and reprogramming them to better search for and kill cancer. These immune cells are modified to contain a protein known as a chimeric antigen receptor (CAR), which targets the CD19 protein found on the surface of cancerous B cells. After the immune cells are collected and re-engineered, the cancer patient has to undergo chemotherapy to wipe out their current immune system before they are re-infused with their newly empowered immune cells.
The research team is working hard to figure out why that group's modified T-cells did not expand in their bodies at the same rate as in those who went into long-term remission. Lead author David Porter, director of Blood and Marrow Transplantation in Penn's Abramson Cancer Center, said, "The patients in this study are pioneers, whose participation has given us a foundation of knowledge and experience on which to build this new approach to help more patients."
Senior author Carl June, professor of immunotherapy in Penn's department of pathology and laboratory medicine, said, "Our tests of patients who experienced complete remissions showed that the modified cells remain in patients' bodies for years after their infusions, with no sign of cancerous or normal B cells. This suggests that at least some of the CTL019 cells retain their ability to hunt for cancerous cells for long periods of time."
The findings are published in Science Translational Medicine.
Advertisement