‘Using the Lung Cancer Risk Assessment Tool can reduce the number of lung cancer deaths.’
Tweet it Now
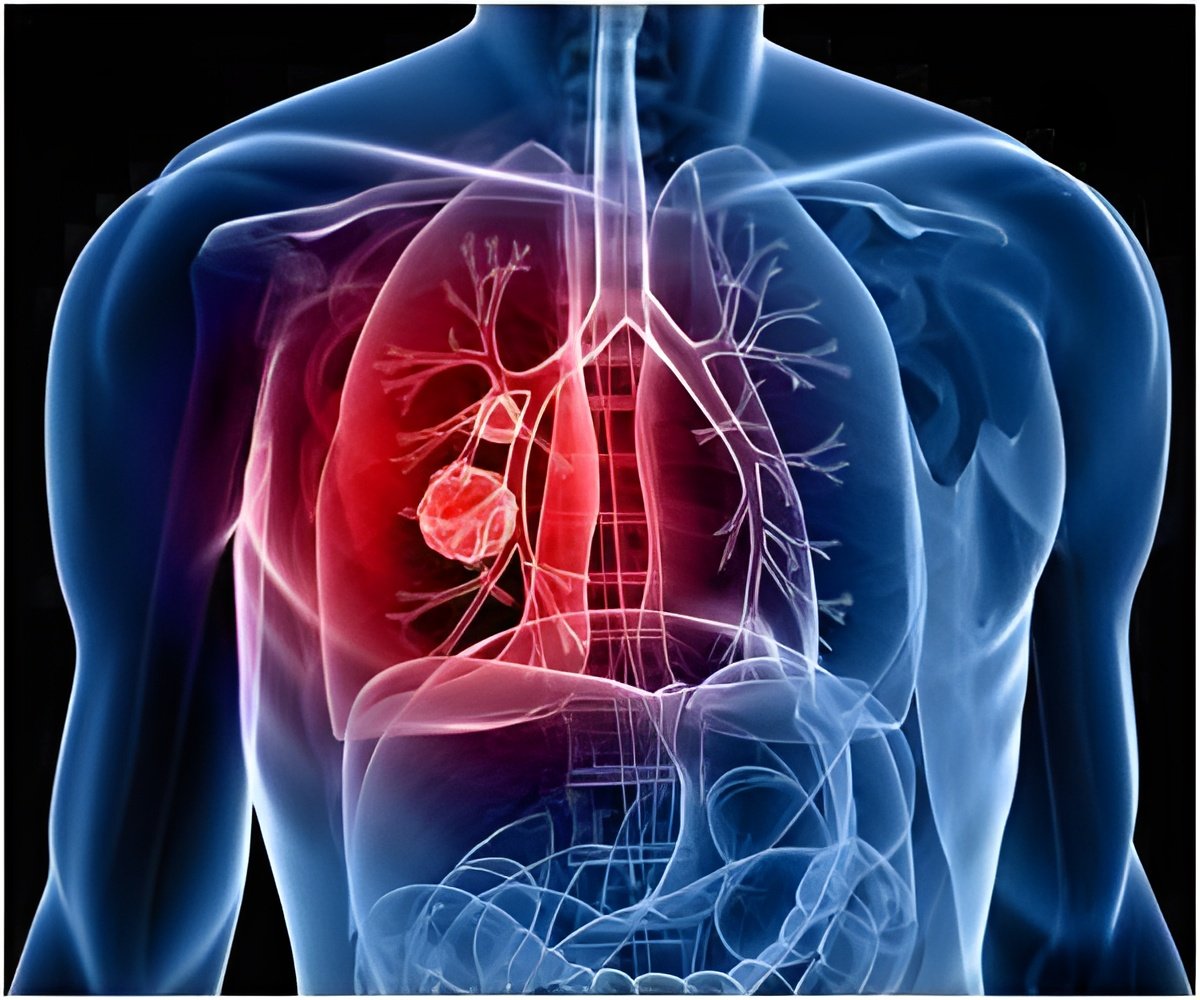
The USPSTF recommends annual lung cancer screening with low-dose computed tomography (CT) for persons aged 55 to 80 years who currently smoke or quit within the past 15 years and have at least a 30-pack-year history of cigarette smoking. These criteria may miss smokers at high risk for lung cancer who would have been selected for CT screening by individual risk calculators that more specifically account for demographic, clinical, and smoking characteristics.
Researchers from the National Cancer Institute used data from the National Health Interview Survey to compare USPSTF eligibility criteria with individualized, risk-based eligibility and estimate the effect of eligibility on lung cancer deaths preventable by screening since 2005.
They found that using the Lung Cancer Risk Assessment Tool would draw in high-risk moderate smokers with a history of 20 to 29 pack-years who are currently ineligible for screening using USPSTF criteria.
This approach could have prevented over 5,000 more deaths in 2015 than using the USPSTF screening criteria. Because of the U.S. population changes related to smoking between 2010 and 2015, adhering to the USPSTF criteria led to fewer ever-smokers being eligible for CT screening and fewer lung cancer deaths being averted by screening.
Advertisement
Source-Eurekalert