Self-testing for Human Papillomavirus (HPV) is as effective at detecting cancer as a conventional smear test (cytology screening) even when scaled up to test large populations.

However, when self-testing was rolled out on this scale, the number of women referred to clinics for follow-up tests rapidly increased. The findings revealed the quality of clinical care then went down, as clinics were unable to handle the high number of patients.
Attila Lorincz, Professor of Molecular Epidemiology and lead author, Queen Mary University of London, Barts and The London School of Medicine and Dentistry, comments:
"Our findings show that large-scale HPV screening can be successfully implemented by home testing. However, if a positive result is received, it's imperative that all other follow-up services are strengthened so they can accommodate the big increase in screened women. This is one of the huge challenges we face in developing countries like Mexico and will continue to work on.
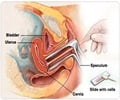
"Cervical cancer is hard to treat and sadly very deadly – but it is also highly preventable. In the UK every woman should be screened for cervical disease by visiting their GP, but if they cannot or will not do this, then we recommend requesting a self-testing device so they can have an HPV test at home."
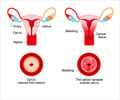
Despite established smear testing programmes in Mexico, cervical cancer rates remain high. This study, published in the International journal of Cancer, shows self-testing works as an alternative to smear testing when rolled out in a large scale and could be particularly beneficial in countries shown where smear testing programmes are poor. In addition, self-testing is desirable because it poses fewer barriers to access for women living in areas with little access to health services.
 MEDINDIA
MEDINDIA


 Email
Email