The total hospital cost of mitral valve repair surgery, from the time a patient is admitted to the hospital until release is similar, whether performed through small port incisions using robotic equipment or via the conventional open-chest method.
"These results reflect an important opportunity to decrease cost and improve quality of U.S. health care when technologically complex procedures are performed by well-trained, high-volume teams capable of leveraging the potential of less invasive approaches for patient benefit," says lead author Rakesh Suri, M.D., D.Phil., a cardiovascular surgeon at Mayo Clinic in Rochester.
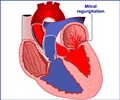
Patients undergo mitral valve repair surgery for severe mitral valve regurgitation, a common condition that is increasing in frequency. By 2030, an estimated 5 million Americans will have moderate to severe mitral valve regurgitation. The condition occurs when the mitral valve does not close properly, causing blood to be pumped backward instead of forward. Oxygen-rich blood is thus unable to move through the heart to the rest of the body as efficiently.
In robot-assisted cardiac operations, small incisions are made on the right side of the chest, and the surgeon conducts surgery using a robotic telemanipulator system, which includes a high-definition camera and thin mechanical arms that act as extensions of the surgeon's eyes and hands. In open-chest surgery, the surgeon cuts down the center of the chest along the breastbone to expose the heart.
"There is concern that the adoption of new technology in the operating room will increase costs," Dr. Suri says. "That does not need to be the case. While total hospital costs were slightly higher initially for robot-assisted mitral valve repair surgery, we found that with increased experience and changes in our care processes, there was a steady and significant decrease in costs over time as we progressed through the learning curve."
In this study performed between July 2007 and January 2011, 370 patients who underwent mitral valve repair surgery (185 robotically and 185 open-chest) were compared. All patients had successful surgeries and there were no early deaths. Halfway through the study period, in 2009, systems innovations were implemented, such as increased efficiency in the operating room and expedited postoperative recovery efforts that allowed patients who underwent robotic repair to have their breathing tube removed in the operating room. They also were more likely to be able to move to a hospital room the day of the surgery, decreasing the time spent in a more expensive intensive care unit.
The length of hospital stay consequently decreased in the patients who had robotic repair surgery. In the pre-systems innovation period, these patients were in the hospital for an average of four days, compared with an average of 5.6 days for open-chest patients. In the post-improvement period, the time frame was 3.7 days compared with 5.7 days, respectively.
The Mayo Clinic Proceedings study follows a Mayo Clinic study in The Annals of Thoracic Surgery in 2012, which found that robotic repair patients returned to work quicker than open-chest patients (33 days and 54 days, respectively). In addition, robotic repair was associated with slightly improved quality of life indicators compared with open-chest surgery during the first weeks after surgery, but indicators became indistinguishable by one year.
Source-Newswise
 MEDINDIA
MEDINDIA



 Email
Email







