A large study shows women who give birth to multiple babies following IVF treatment are at a higher risk of breast cancer than those giving birth to singletons or who remain childless.
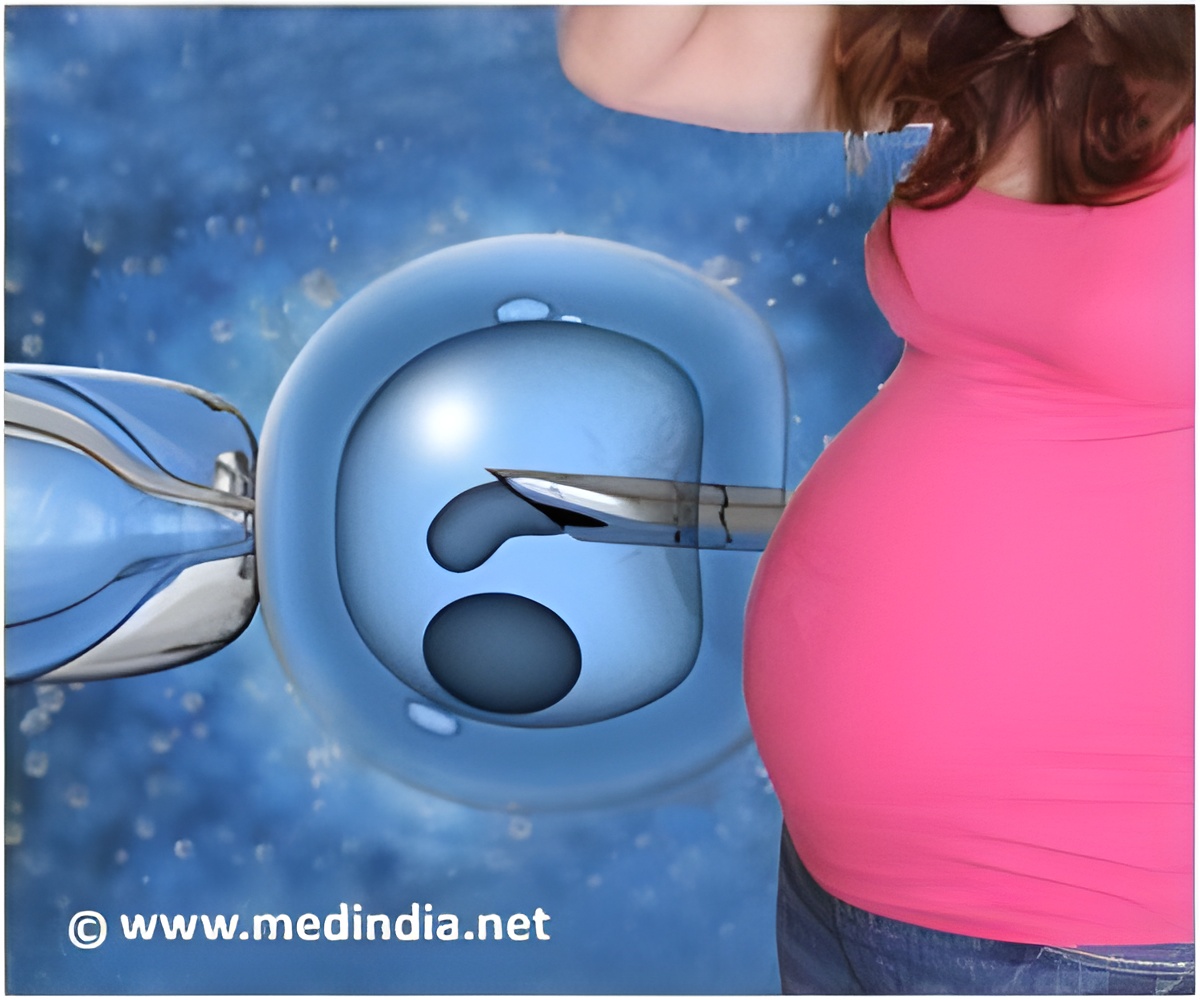
Although the results were derived from a large nationwide cohort study, the investigators emphasise that the findings should next be replicated in further studies and that presently there is no reason for earlier breast cancer screening than is recommended for the general population.(1)
The study, presented today at the annual meeting of ESHRE by Dr Els Groeneveld from the VU University Medical Centre of Amsterdam, the Netherlands, analysed data from the Omega study, a large Dutch nationwide cohort of 19,861 women who received IVF or ICSI treatment between 1983 and 1995. Between 1997 and 1999 all patients were questioned (by questionnaire) about their treatment and its outcome. Those who completed the questionnaire (12,589 women) were cross-referred to the Netherlands Cancer Registry.
Cohort analysis showed that over a median 16.7 years of follow-up 1688 women in the study gave birth to multiples (13%), 6027 delivered singletons (48%), and 4874 remained childless (39%). Among these women there were 317 confirmed diagnoses of breast cancer, of whom 57 gave birth to multiples, 155 to singletons, and 105 remained childless. When these findings were analysed statistically, results showed that mothers of multiples had a (44%) higher breast cancer risk than the mothers of singletons (hazard ratio 1.44, statistically significant) when adjusted for year of IVF treatment, number of IVF cycles, height and age at first birth. Nulliparous women were at no increased risk of breast cancer.
Remarkably, only multiple pregnancies conceived after the complete implantation of all transferred embryos were associated with an increased breast cancer risk (HR 1.86), whereas multiple pregnancies conceived after incomplete implantation were not (HR 1.31, not statistically significant). This finding, says Dr Groeneveld, supports the hypothesis of a link between high embryo implantation potential and breast cancer risk.
She explained: "It has been generally assumed that increased levels of estrogen and progesterone in multiple pregnancies stimulate cellular proliferation in the breast, which increases accumulation of somatic mutations during cell division and leads to the development of breast cancer. Thus, breast cancer could be seen as a consequence of the multiple pregnancy itself. However, we also hypothesise that an additional maternal trait might be associated with an increased breast cancer risk in these women."
"In our study women who developed a multiple pregnancy from all transferred embryos represent women with high embryo implantation potential, possibly through increased levels of VEGF," said Dr Groeneveld. "Future studies will reveal whether the significant association between improved embryo implantation potential and breast cancer risk shown in our study is actually based on increased levels of VEGF. "So the main message of our study is that the increased breast cancer risk is not only a consequence of the multiple pregnancy itself because of high hormone levels, but that the risk of breast cancer may already be elevated prior to conception in women who have the potential -- the 'maternal trait' -- to develop a multiple pregnancy from all transferred embryos."
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email