A new study reports on the discovery of a novel mutation in hepatitis B virus seen only in men which makes it five times more likely that HBV-infected men develop liver cancer.
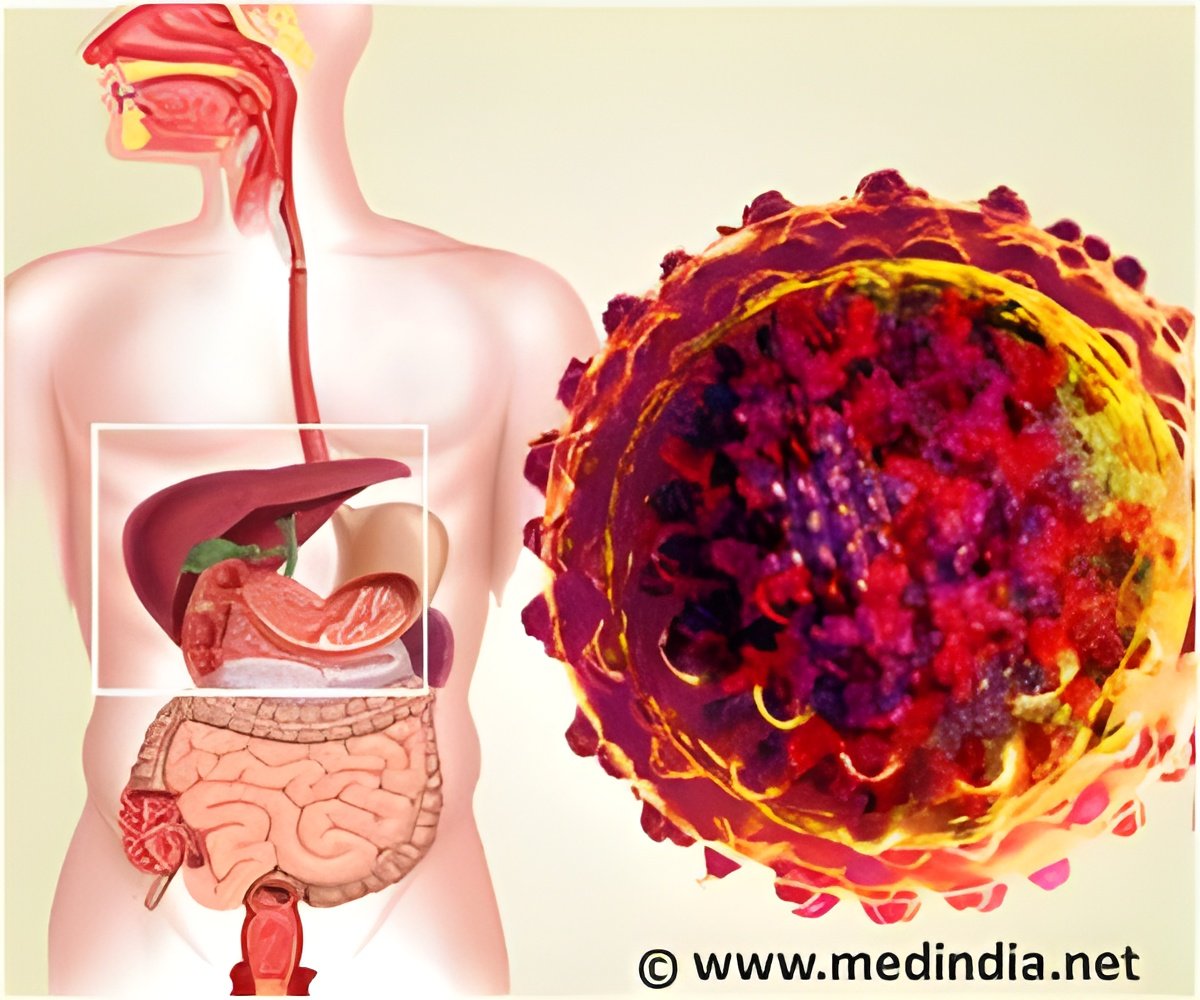
In the study, the researchers randomly collected and analyzed serum samples from 292 patients with chronic HBV infection who visited one of 3 hospitals in Korea from 2003-2005. Previous studies had suggested that a gene mutation known as W4P/R was associated with higher incidence of liver cancer and cirrhosis. They developed an assay to specifically identify HBV with the W4P/R mutation. When compared to patient outcomes, the W4P/R mutation was significantly associated with severe liver disease and was found exclusively in male patients.
The investigators believe the assay they developed to discover the mutation may hold promise as a diagnostic for predicting male progression to cirrhosis and liver cancer. They caution that first larger studies are necessary to confirm their findings, as only 67 of the 292 samples came from women.
HBV infection is a global health problem, with 350 million chronic carriers of the virus, a number that is roughly equivalent to the combined populations of the US and Canada. The prevalence of infection ranges from less than half a percent in the United States to around 10 percent in Asia, to as high as 15 percent in parts of Africa. Major means of transmission include injection drug abuse, unprotected sex, and transmission via childbirth. Worldwide mortality is about 600,000 annually, according to the World Health Organization. In the US, despite the availability of a vaccine, an estimated 3,000 die annually from hepatocellular cancer or chronic liver disease caused by hepatitis B.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email