An increase in liver enzymes and fatty liver is associated with pre-diabetes and diabetes.
The study was conducted on 3009 individuals that included 1556 females and 1453 males aged between 32 to 81 years.
A person in the study was said to be pre-diabetic if certain blood glucose tests were abnormal, that is, the person showed impaired glucose tolerance test (IGT) or fasting blood glucose (IFG), or both. Some of the participants had known or newly diagnosed diabetes. Blood glucose levels, HbA1c and C-reactive protein levels were estimated in all participants.
Liver function was estimated by checking for liver enzymes like gamma-glutamyltransferase (GGT), glutamate-pyruvate transaminase (GPT), glutamate-oxalacetate transaminase (GOT) and alkaline phosphatase (AP). The fatty liver index, that is, Bedogni Fatty Liver Index (FLI), was also calculated and a score of greater or equal 60 points was considered as positive for fatty liver disease.
Other information on socio-demographic variables, smoking habits, physical activity, medication use, alcohol consumption, household characteristics, educational attainment and physical activity were also collected. The participants were also examined for waist and hip circumferences measurements, body mass index, blood pressure and had to undergo blood testing.
Among the participants included in the study, 229 participants reported known diabetes, 106 had newly diagnosed diabetes, 107 had IFG, 309 had IGT, 69 were had both IFG as well as IGT, and 74 could not be classified (due to inconsistent information regarding diabetes status or glucose tolerance test could not be successfully conducted due to various reasons).
The study also inferred some other findings. Briefly, these are:
• More males suffered from glucose disturbances
• A number of individuals with less than 10 years education had IGT, newly diagnosed diabetes or known diabetes.
• People suffering from pre-diabetes and diabetes had higher body mass index, waist, hip circumference and high blood pressure.
• Pre-diabetics had a higher value of total cholesterol.
• People with glucose disturbances had higher values of triglycerides, CRP, HbA1c and uric acid.
• People with known diabetes had lower alcohol intake
• Smoking was less common in patients with IFG
• People with known diabetes were physically less active during their leisure time
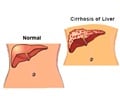
Patients with pre-diabetes and diabetes had higher incidence of fatty liver, as estimated using the fatty liver index. People taking diabetes medication showed a decreased association between diabetes and fatty liver, indicating a beneficial effect of diabetes medication on fatty liver.
The study thus indicates that increase in liver enzymes and fatty liver is associated not only with diabetes, but also with pre-diabetes, as defined by an impaired fasting glucose or impaired glucose tolerance, or both. These enzymes could thus be used as inexpensive and easily available early indicators of abnormal glucose metabolism.
Reference:
1. Association between Markers of Fatty Liver Disease and Impaired Glucose Regulation in Men and Women from the General Population: The KORA-F4-Study; Ina Maria et al; Plos One 2011.
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email










