Live Donor Kidney Transplantation results can be improved by pretreatment with plasmapheresis and immune globulins prior to transplantation.
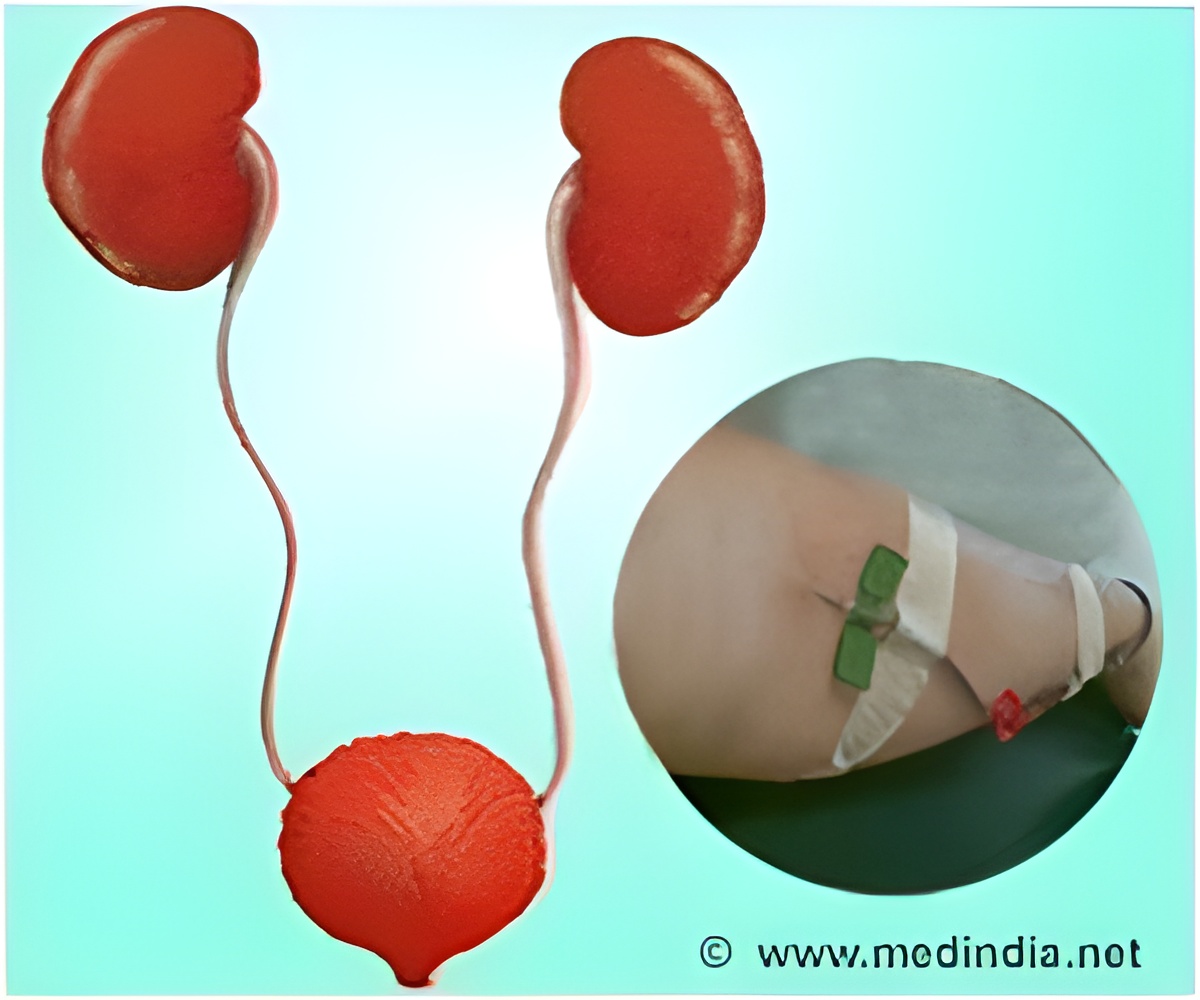
The Johns Hopkins Medical Institutions developed and tested one such pretreatment to permit transplantation in patients having anti-HLA antibodies against the donor, and thus at a high risk for rejection. In this procedure, kidney failure patients initially underwent plasmapheresis i.e. a process through which antibodies that could react against the transplanted kidney were removed from the blood. After each session, patients were injected with intravenous immune globulin. The number of treatments depended upon the baseline level of donor-specific anti-HLA antibodies. This process conditioned the patient’s body to accept the transplantation. Out of the 215 patients who underwent this process, 211 proceeded to transplantation. The patients received at least two plasmapheresis sessions after the transplantation as well. As with normal transplantation procedures, drugs that suppress immunity were administered in addition before, during and after transplantation.
The researchers found that with this approach, the survival rates in the kidney transplant patients were 90.6% at 1 year, 85.7% at 3 years, 80.6% at 5 years and 79.7% at 8 years. The survival rate at 3, 5 and 8 years was much better than patients who continued on dialysis (dialysis-only group) or those receiving dialysis, some of whom underwent transplantation with an HLA-compatible kidney during the study (dialysis-or-transplantation group).
In the study, the plasmapheresis procedure was associated with minor adverse effects. Anaphylaxis or a severe allergic reaction occurred in 3 patients. Some patients suffered from excessive bleeding, which could have been associated with plasmapheresis.
The researchers thus claim that pretreatment of renal transplant patients with plasmapheresis and low dose immune globulin permits transplantation in patients with anti-HLA antibodies against the donor kidney. These patients in addition show better survival as compared to patients continuing on dialysis while waiting for a matched transplantation.
This research thus provides good news for patients who have a willing but non-matching donor. The desensitization procedure will permit such transplantations and hopefully reduce the waiting list of people in need of a matched kidney transplant.
Reference:
Source-Medindia
 MEDINDIA
MEDINDIA

 Email
Email