At Emory and Georgia Tech, researchers have developed a potential treatment for atherosclerosis that targets a master controller of the process.

In a twist, the master controller comes from a source that scientists had thought was leftover garbage. It is a micro RNA molecule, which comes from an unused template that remains after punching out ribosomes –– workhorse protein factories found in all cells.
The treatment works by stopping the inflammatory effects of disturbed blood flow on cells that line blood vessels. In animal models of atherosclerosis, a drug that blocks the micro RNA can stop arteries from becoming blocked, despite the ongoing stress of high-fat diet. The micro RNA appears to function similarly in human cells.
"We've known that aerobic exercise provides protection against atherosclerosis, partly by improving patterns of blood flow. Now we're achieving some insight into how," says senior author Hanjoong Jo, PhD. "Healthy flow tunes down the production of bad actors like this micro RNA. Targeting it could form the basis for a therapeutic approach that could be translated with relative ease compared to other drugs."
Jo is John and Jan Portman professor in the Wallace H. Coulter Department of Biomedical Engineering at Georgia Tech and Emory University. The co-first authors of the paper are postdoctoral fellows Dong Ju Son, PhD and Sandeep Kumar, PhD.
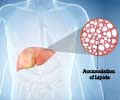
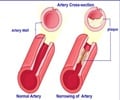
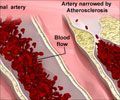
In atherosclerosis, arterial walls thicken because of a gradual build-up of white blood cells, lipids and cholesterol. The process can lead to plaque formation, and eventually to heart attacks and strokes.
Jo and his colleagues have developed an animal model where it is possible to drive the development of atherosclerosis quickly and selectively, by partially restricting blood flow in a mouse's carotid artery. To accelerate the process, the mice also have a deficiency in ApoE, important for removing lipids and cholesterol from the blood, and are fed a high-fat diet. The model allows researchers to compare molecules that are activated in endothelial cells, which line blood vessels, on the disturbed side versus the undisturbed side in the same animal.
In response to disturbed or unhealthy blood flow, endothelial cells produce miR-712, the researchers found. miR-712 in turn inhibits a gene called TIMP3, which under healthy flow conditions restrains inflammation in endothelial cells.
The researchers were surprised to find that miR-712 comes from leftovers remaining from a long RNA that is used to form ribosomes. Ribosomes are ubiquitous and perform the basic housekeeping function of protein assembly.
"This is one of the most abundant streams of RNA that cells produce, and it turns out to be the source for a molecule that controls atherosclerosis," Jo says. "Why did nature do it that way? I don't think we know yet."
By using a technology called "locked nucleic acids," Jo and his colleagues tested the effects of blocking miR-712 in the body. When given to mice in the rapid atherosclerosis model, the anti-miR-712 drug inhibited the development of arterial blockages. Without the drug, plaques blocked an average of 80 percent of the disturbed carotid artery, but the drug cut that in half. The drug worked similarly in another model of atherosclerosis where animals develop disease more slowly.
Locked nucleic acids that target an unrelated disease (hepatitis C) are being tested in clinical trials, and so far appear to be effective. A micro RNA similar to miR-712 appears to have the same inflammatory control function in human endothelial cells; it's called miR-205.
Jo says his team is devising ways using nanotechnologies to deliver anti-miR-712 drugs to the heart or to endothelial cells specifically to achieve efficient therapeutic effect with minimum side-effects.
"It is notable that in our experiments, the anti-miR-712 drug was delivered systemically, but still made its way to the right place and had a strong effect," Jo says. "This is a good sign for future translational studies."
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email