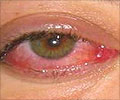
According to a new study funded by the National Eye Institute (NEI), the age of the donor is not a factor when it comes to corneal transplants

The Cornea Donor Study found that 10-year success rates remained steady at 75 percent for corneal transplants from donors 34 to 71 years old. It also found slightly higher success rates for donors under 34, and somewhat lower rates for donors over 71.
In the U.S., three-fourths of cornea donors are within the 34 to 71 age range, with one-third of donors at the upper end of the range, from 61 to 70 years old. When the study began in 2000, many surgeons would not accept corneas from donors over 65.
"The findings clearly demonstrate that most corneal transplants have remarkable longevity regardless of donor age," said Mark Mannis, chair of ophthalmology and vision sciences, director of UC Davis Health System's Eye Center and co-chair of the study. "The majority of patients continued to do well after 10 years, even those who received corneas from the oldest donors."
The Corneal Donor Study "supports continued expansion of the corneal donor pool beyond age 65," said study co-chair Edward J. Holland, professor of ophthalmology at the University of Cincinnati and director of the Cornea Service at the Cincinnati Eye Institute.
Corneal disease and study design
The supply of corneas does not meet the demand internationally, and as the aging population grows at home and abroad, the need for corneal transplants is expected to grow, too. The Cornea Donor Study was designed to address whether making use of donor corneas across the full range of ages available might help solve this problem," said Maryann Redford, a clinical research program director at NEI.
About two thirds of patients had an inherited corneal disease called Fuchs' dystrophy, and one third had corneal swelling after cataract surgery. These conditions involve loss of cells in the innermost (endothelial) layer of the cornea and are leading reasons for corneal transplants reported to U.S. eye banks. Graft failure was defined as the need for a new transplant, or a cloudy cornea that caused blurred vision for at least three months.
The investigators originally planned to follow patients for five years post-transplant. In 2008, they reported that the five-year success rate was identical — 86 percent — for transplants from donors aged 12 to 65 and those aged 66 to 75. However, when the investigators examined endothelial cells in the transplanted corneas, they found that older corneas had a slightly higher rate of cell loss. Higher cell loss at six months also predicted a higher likelihood of graft failure at five years. That prompted an expansion of the study to determine if donor age would affect transplant viability 10 years after the procedure.
Findings at 10-year mark
During the follow up, 663 participants remained eligible and willing to continue with the study. The investigators report that at 10 years, the transplant success rates for corneas from donors aged 12 to 65 and aged 66 to 75 remained similar, at 77 percent and 71 percent, respectively. However, when the investigators separated the donors into smaller age groups, they found some differences. The success rate remained steady at 75 percent for the vast majority of donors ages 34 to 71. But it increased to 96 percent for donors age 12 to 33 and decreased to 62 percent for donors age 72 to 75.
The investigators also re-evaluated the endothelial cells lining the inner cornea in a subgroup of 176 patients who had a successful transplant at 10 years and for whom high-quality images of the cells were available. The data confirmed the trend in cell loss seen at five years. At 10 years, corneas from donors over age 65 had a slightly higher rate of endothelial cell loss (79 percent) compared to those from donors age 65 and under (76 percent). The youngest corneas, from donors age 12 to 33, had the highest number of cells before surgery and the lowest rate of cell loss at 10 years (67 percent).
"The cell loss data parallels the graft survival data, but we don't yet know if a given number of cells at five years is predictive of graft failure at 10 years," said Jonathan Lass, professor of ophthalmology at Case Western Reserve University and University Hospitals Case Medical Center in Cleveland and medical director of the study's cornea image analysis reading center. That analysis is being done and will be released at a later date, he said.
Penetrating vs. endothelial keratoplasty
The investigators note that corneal surgeries have changed in the past decade. Penetrating keratoplasty was the standard procedure used for corneal transplants when the study was launched. But today, most patients with Fuchs' dystrophy or corneal swelling undergo endothelial keratoplasty, which involves replacing only the endothelial layer rather than the entire central cornea. The ongoing Cornea Preservation Time Study (NCT01537393), led by Lass and also funded by NEI, is examining the factors contributing to transplant success after endothelial keratoplasty. In the meantime, the investigators say the current study provides the most comprehensive data on the relationship between donor age and corneal transplant outcome.
Given the high success rate for transplants involving young donors (under age 34), the investigators wrote that their analysis "raises the question…of whether age-matching of donors and recipients is appropriate at the extremes of recipient age." Such age-matching is already a frequent practice for children and other young patients in need of corneal transplants, who routinely get corneas from young donors. But young donor corneas are relatively rare. In 2012, corneal donors under age 31 comprised less than 10 percent of the U.S. donor pool.
Surgeons often seek the youngest corneal tissue available regardless of patient age. Historically, some surgeons set extremely restrictive upper age limits, even refusing tissue from donors over age 50, Mannis said.
"The study demonstrates the viability of older donor tissue in the majority of cases with endothelial disease," he said. "In time, we hope the study will have a lasting impact on the practice of corneal transplant surgery. Although the results suggest that age-matching may be appropriate for the very youngest donors and patients, we do not think it is necessary in the vast majority of cases."
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email